Just got news of my sixth go-round with renal cell carcinoma – kidney cancer. I haven’t blogged for ages. I thought I might blog daily, until this one is done, mostly to try and communicate the rollercoaster that is living with cancer.
They’ll mostly be quite short, I think.
Newest posts are at the top; older ones underneath.
Day 34: Ablation Day +1 (Wednesday 25th April)
The prisoner ate a hearty breakfast, and eked out her diminishing stash of peppermint tea by re-using the teabag from the 6am drinks round. You are offered tea, coffee and other drinks pretty constantly in hospital. I think it’s part of a bid to stop patients becoming dehydrated. But it’s more tea than I want, and the coffee’s no good because I’m a coffee snob, and can’t drink instant any more. At 10am when I declined a drink the woman gave me a really dirty look, as if to say ‘Well, be it on your own head..’
I’m feeing good. I’m a bit sore round the kidney, but otherwise feel weirdly normal. I have a shower, and punt up and down the long ward corridor a couple of times, just to get the juices flowing a bit.
I’ve been smug so far about my blood glucose. I’d replaced my pump once I was back on the ward last night, although I don’t really remember doing it, and over night my glucose has been very good. But now it’s starting to ramp up as a reaction to the physical trauma of the ablation. I increase my background insulin by about 25% and keep an eye on it.
Mrs In-The-Bed-Opposite got very upset several times through the morning, as nurses variously tried to give her breakfast, change her, change the bed, wash her and do her obs. She accused one guy of ‘going in her bum, and having his fun’. This is heartbreaking stuff. I’m sure that this woman is/was fundamentally bright and engaging person who has had a full and busy life, but now she’s a sort of angry shell of her former self. She refused lunch, too, several times, but eventually agreed to eat a yoghurt, which she complained bitterly about.
Kate, my Oncologist, visited. We’ve known each other since 2003 when I first got secondaries and I think we count as friends. We chatted quite a lot. Talked about the wedding arrangements and my frock. We also talked about my cancer, and some of the various scenarios that might arise in the future. A friend in Oxford is involved in some research that might help at some point, but not yet. I have no idea whether Kate goes to see other patients when they’re in hospital. Either way, it’s a nice thing to do, and it was lovely to see her. We laughed a lot, and I got a big hug.
Interestingly, Kate told me that this ward, D7, was actually the urology ward until last week, since when it has become a medical ward (hence the old ladies with dementia, falls and so). However, although the urology patients are now in a shiny new ward across the campus, the urology staff don’t move until next week. So actually, these urology specialists are doing especially well with the dementia patients.
The porters arrived just after lunch, to take me for my CT scan. The porter was puzzled about ‘where the back of my chair was’. It does have a back about 20cm high, but he’s worked so long with the great hospital wheelbarrows, that he assumed mine must have another folded away somewhere. And ‘where were the handles?’
We got half way down the corridor before I panicked and realised I hadn’t got anything to read. I’ve waited for two hours in the inpatients’ CT waiting room before. Nick the Porter was dubious, and a bit worried about time, but I shot back.
Miltos came out to the CT waiting room to say hi and to let me know that we wouldn’t be long. We weren’t. The CT didn’t take long, and he was soon out of the control room to say that the pneumothorax was still visible but obviously healing and resolving, and that the kidney looked good – no bleeding or other problems. He was happy for me to be discharged, and said that he would email the ward straight away. Great news!
We chatted for a bit about the awful postural position that patients need to adopt for the ablation, due to the fact that the CT bed is designed for patients to lie on their backs. Barb’s cushions and pillows had actually saved my neck and shoulders from being much more sore than they were. It wouldn’t be too difficult to put a range of cushions in the CT suite, to suit different shapes and sizes, would it? And I suggested that it might be useful to have a Physio come and look at the set up, and make some suggestions. Miltos seemed to think this was a surprising, but good, idea, and appeared receptive to it. Must remind him.
He said that he’d make another CT appointment for 4 weeks. He could do it now, here on the spot, but if he did, at the point that I was discharged this afternoon, the CT scan would be deleted. Systems!
I made my own way back to the ward, via Costa, and took my coffee back to the ward, where I let them know that Miltos said I was good to go. I put a new pump on again, because I’d had to take last night’s off for the CT scan again. Glucose is still very high (about 19mmol/l) so I rack up the background insulin again, to about 150% of normal, to see if that has the required effect.
A pharmacist appeared, and double-checked that I didn’t need any meds to take home. And I called H to tell him that I’d be coming home at some point. I’d let him know once I’d go the discharge letter in my sweaty little hands, otherwise you can spent months waiting for that…
Soon afterwards, Justine phoned to say that she had a meeting in the hospital, and could pop up afterwards if I were up for it. Oh my, how splendid. I was definitely up for it! It was fantastic to see her. We’ve known each other since 2012, and both have long histories of cancer, and surgeries you don’t want the details of. We ‘get’ what it’s like for each of us. She didn’t bring me grapes though.
Eventually the discharge letter is here, and I call H, who turns up pretty quickly. I’m eating my ‘tea’ as he arrives. Meal times in hospital are SO weird. Who has their tea at 4.30pm?
It’s great to be home, with H, and I lie on the sofa and love it. There’s a G&T. Not the violet one. That’s tomorrow.
Day 33: Ablation Day, Part 2 (Tuesday 24 April 2018)
———————————————————————————————————-—-———Sorry for the radio silence. I have been – and remain – very, very knackered, and what energy has been used has been spent on our basketball club’s fundraising day on Saturday, and with family and friends over the weekend. The next few posts after this will be short as I catch up.
————————————————————————————————————————-
Woke after the procedure (Radiofrequency Ablation, or RFA) at what must have been about teatime with a lot of pain and sickness, and very, very dozy and bleary. After a while I noticed that my basketball friend Eve was there. She’d come up after finishing work in the Eye Unit, and sat there humouring me as I drifted in and out of sleep, and talked a stupendous amount of nonsense.
I’d had a couple of doses of Fentonyl at the start of the procedure and then as the actual cooking started. I don’t do well with any opiates; they all make me vomit, some have given me hallucinations (both hilarious and deeply disturbing and frightening), and they keep me dozy for days and days. I’ve read recently that weight-for-weight, and depending on how it is produced, Fentonyl is between 75 and 10,000 times as strong as morphine. So I’m assuming it was a teeny tiny amount. But nevertheless, I’m reeling. I could actually hear myself starting a sentence, and getting lost in the middle, then finishing it on some other topic completely. Dozing off mid sentence…
Eve took it on the chin. Eve is cool.
I was in a lot of pain, round my kidney, and the area on my back where the needles had gone in, and there’d been the pushing and pulling. And I had a terrific pain in my upper right back too, and was chucking up fairly regularly. It was rough, really. And I’m sure it was pretty hard for H too. I think I had some IV paracetamol at some stage, which helped. Yeah, I can see the empty bag in my mind’s eye.
Miltos appeared in the early evening, and was reassuring, and fairly optimistic about how it had gone. We won’t know for sure until after a CT scan in a month. He said that there had been a pneumothorax, though: a fairly common complication of the procedure, and this explained the pain in my back! A pneumothorax is a ‘penetrating chest wound’ (this was the needle catching the diaphragm and puncturing it on the way to the kidney). This means that air gets into the space round the lungs and the pressure on the lung leads to its partial (or indeed complete) collapse. This was a known risk, particularly when getting into the middle of the kidney.
Because it’s a single small hole, he was optimistic that it would seal itself, but we would know after the CT scan in the morning.
I did say earlier on that this procedure is a kind of ‘controlled stabbing’.
I continued being kinda stooped. Eve rang H to say I was back on the ward, and at some point she wasn’t there and Howard was. Heroically, and perfectly, he’d brought my little bear into hospital, and it was nice to snuggle down with him.
At some stage the cannula came out and my elbow bled, on me and the sheets and on the bear too, I discovered later.
I remember a nurse coming and saying that they’d replace the cannula. And the next nurse coming and when I asked if she was putting a new one in, she asked why I needed one. God knows, I thought. I started to formulate ‘Well, the other nurse said…’, but I shut up. I couldn’t be arsed arguing the toss at this stage.
For those of you who know me, this does suggest that I was in quite a state!!
H sat with me as long as he was allowed, and left, telling me to ring him during the night if I needed a chat. I went back to sleep.
I woke up later, a bit confused and feeling as though I’d slept for a whole night, but I was puzzled about it still being dark. It turned out to be about 10.30pm. I feel much better. There was still a pain in my kidney, but the much worse pain in the top of my back was gone.
A nurse appeared to do my obs, and offered my tea and toast and paracetamol. Ooh, yes please. Never has soggy white toast tasted so marvellous, and it stayed down.
Shortly afterwards, as the nurses approached the woman opposite to do her obs, she started raving and shouting. She had dementia, and couldn’t understand what the nurses were doing or why. She repeatedly shouted ‘Get your hands off me!’ And then she screamed — properly, loudly — for about five minutes, and argued about why they didn’t need to change her bed (they really did). She wouldn’t let them touch her to roll her over: ‘I can do it myself’. Okay, would you please roll over?’ ‘No! I don’t want to! I don’t want you changing my bed.’ But we can’t leave you on wet sheets…’
So our bay was awake and so were most of the others on the ward. The nurses were genuinely heroic: they were patient and kind and explained over and over what they were doing. They tried different approaches and arguments. They kept asking her to roll over, and asked permission every time they needed to touched her. It was all a bit hopeless, of course, and it was repeated at every intervention, all night.
The staff here – nurses, healthcare assistants and various ancillary staff, have all been pretty good. The only ‘fail’, as the young people say, is that they have failed consistently to introduce themselves. I don’t know why. I asked over and over again, and they’re usually happy to tell you, but I’m mystified as to why this isn’t rammed into them in training, and by the senior ward staff. It’s cheap, it takes no time, and it makes all the difference in the world.
Eleven fifteen-ish. I’m off up the wooden hill.
Day 33: Ablation Day, Part 1 (Tuesday 24 April 2018)
Awake early, overnight gear all packed, and away to Addenbrooke’s in good time.
Grace, a nurse in the Radiologist Day Unit welcomes me by name and says she remembers me from before, and reminds me which bed I was in, in the window corner. Amazing. It feels like coming home!
Admission: labels, questions about allergies, my GP, phone numbers, cannula in, bloods taken, small conversations with the other prisoners.
Howard waits around for a bit then, when I’m settled in, he goes home.
At this point my phone pings and a message from MyChart (the Patient-accessible part of the records system at Addenbrooke’s) tells me that an appointment has been re-scheduled. Surely not this one? Now?
Nope. It’s a different thing: a follow-up appointment for a benign lesion behind my left eye.
• The original date was November, and I had to postpone it because of our trip to New Zealand.
• The new appointment was in December, but it was cancelled and moved to February.
• The February one was cancelled and moved to April.
• The April one was cancelled and moved to June.
• Today’s ping was the June appointment being cancelled and moved to August, now nine months after the original date. And we won’t be here. Great.
I can deal with this later.
Then Grace comes to say that she wants to keep me in the picture about ‘the situation’. Oh dear. The situation is that she’s been checking round on the bed front, and there is pretty much zero chance of getting a bed in Urology for the night. They are all taken, and no-one is going home. There is a small chance of a bed on a medical ward, but it’s really quite small. So, even though I’m undressed and cannula’d up, it’s very unlikely that this procedure is going to happen. She’s very apologetic, and goes back to the phones to keep trying.
A bit of me would be relieved, because this isn’t going to be fun. But actually worse was the prospect of having to assuage the indignation of everyone we will have to tell about this. The family, friends, neighbours, who have also been anxious, and will be waiting for news. The thought of having to explain and inevitably defend the situation is appalling.
Eventually, when I’m on the phone to Howard about half an hour later, Grace comes back, pointing at her own ‘big smile’ face and doing a big thumbs up. She’s slept with half the hospital… No! Just kidding. But she told them I’d been nil-by-mouth since 2am and as a diabetic was at risk of having a hypo, which she and I knew wasn’t true, but most people don’t get it. Anyway, whatever. There was a bed with my name on it in D7, a medical ward. Amazing Grace.
Phew. I think.
More prelims
I hear the rumbling voice of Miltos, the Consultant Radiologist. I like him, and I trust him, and he’s a bear of a man. We talk generally about the NHS, how the urology beds are being re-organised, how difficult it is to introduce new and better procedures. He’s working hard, I know. He circles his finger: ‘But I am such a little cog.’ And he is; it’s true. In the scheme of things it’s really difficult to change things. But not to me. Not today. Today, he’s the Man!
We talk about the operation, and the risks, which we’ve rehearsed before. And we get on to the subject of whether we can improve the postural thing. I don’t think doctors think about this stuff much. They are focussed on the tumour, the knee, aortic valve. But it turns out that we’ve both got sore shoulders. And we try to think of ways of relieving the awful pressure on the shoulder joints and arms. I told him that I’ve brought some of Barb’s cushions, and can we try them? ‘Of course,’ he says.
He says that ‘they’ will come for me at about 1pm, and disappears, probably to fix someone else in the meantime, although obviously I hope he’s only thinking about me today, and my tumour.
‘On having your offal cooked while you’re wearing it’
A radiographer and a nurse come for me pretty much as predicted, and we laboriously make our way through bed queues at lifts, and down to the CT suite.
On arrival, I recognise several people who were involved in this last time, and they are friendly and seem to recognise me too, including the anaesthetist, called Sasi, I think. A young radiographer starts to explain something basic about the CT scanner – I can’t remember what – and someone says ‘It’s okay, she knows.’
Not counting the dozens done during these RFA procedures, I’ve had upwards of 70 CT scans.
Next we discuss how we are going to manage my diabetes. The usual route is to set up what is called a ‘sliding scale’ – basically hanging a glucose bag, and some insulin, and have someone test my glucose regularly, and adjust one or the other. The thought of this has always terrified me, because I’m very sensitive to insulin. (When correcting high blood glucose, 1 unit of insulin drops most people’s glucose by 2-3 mmols/l. It drops mine 9.5 mmols/l). So if I had high glucose, and some fool delivered ‘the usual’ corrective dose, I’d be toast. The guys asked about my ratios, and I was impressed that they grasped it. Lots of professionals don’t.
Anyway, in the end we decide not to do the sliding scale set up; that I will decommission my pump; they’ll check my glucose periodically during the procedure and we’ll discuss any adjustments together; and then I’ll put a new pump on as soon as I wake up. Suits me.
So. On with the job. Before I get on the CT bed, Miltos produces a thick, heavy pad, about the size of a paperback. This is the earthing plate. It’s attached to the front of my thigh and, I think, to the base of the CT machine. I’m assuming that it’s there to protect me, but it might be there to save the CT scanner shorting out!
Then I’m invited to get on the CT base. I do. It’s very hard, and I have to lie on my front, and I have bosoms and bony ribs and knees, and I’m gonna be here a while. So I ask for blankets and towels, and we make pads and create gaps to complement my inny bits and outs bits.
Next, there’s a hard plastic headrest raised up at quite an angle, obviously designed to be used by someone lying on their back, not their front. A radiographer throws a couple of pillows on top of it and invites me to lie down. I tell him that there is no way I can lie on that, face down, with my head on its side and bent up at a 20 degree angle. Not and breathe. Not and ever walk again. Not and not scream.
Oh.
I ask if it’ll come off.
Yes!
I ask if we can try Barb’s cushions in the big hollow just revealed, and they’re a bit surprised but there isn’t any reason not to, and someone goes off to rummage in the bag that’s come down with me from the Day Unit. I fiddle with a u-shaped cushion and, using this with the opening off to my right, I can rest my chin and forehead on it and – crucially – breath without having to turn my head completely to its side. Do-able.
It’s still awful. Arms above the head; a blood-pressure cuff on my right arm, with the sharp bits pressing here and there; the cannula in my left arm with two trailing tubes linked up to Fentonyl and, eventually, the contrast agent; then nasal oxygen with the tubes round my neck and, necessarily, lying under my face. Then there are drapes, so I can see through just a peephole.
Bliss.
As everyone starts to settle to their tasks, and they do a summary of the plan, and who’s doing what, and where and when, I feel a small panic rise, and I suppress a tiny sob, hoping they haven’t noticed. Can I do this? Can I hold still under the physical stress? I know how hard this is going to be. No choice, really. Buckle down. Grit your teeth. The finish time can only get closer. I’ve read A Brief History of Time.
‘You okay, there?’ Miltos asks.
‘Yeah, I’m fine. Let’s do it.’
Some Fentonyl goes in through the cannula. Then local anaesthetic, ‘sharp scratches’. I sense a smallgrowing bleariness from the Fentonyl. A scan. Everyone withdraws and it’s just me and the whirring machine. Another scan. Another scratch. Always an apology. I lose count.
Then the bigger, probe-carrying needles, that have to be wiggled up into my kidney, and into the heart of the tumour, preferably bypassing loops of bowel, blood vessels, nerves, as much muscle as possible, and the dome-shaped diaphragm, which apparently curves down a lot at the back. It’s not an easy gig for anyone. Another scan. Me and the whirring. The guys come back.
The anaesthetic means I don’t really feel these needles go in, but I do feel (and hear) enormous pressure on my back and, as the tip is wiggled and moved around (like the head of the Hungry Caterpillar), I definitely feel a slightly gritty, scraping sensation in my kidney. Hmm, slightly gritty. Like if you cut through kidney.
And two or three times there is a shocking bolt of electricity in my back as a nerve is tweaked. I gasp, and grunt, and try not to move. Miltos apologises and sounds like a man who would wish this away if he could. ‘I’m sorry, Fiona,’ he says. ‘It’s okay,’ I say. He concentrates. This is hard.
More scans. More positioning. After an hour the anaesthetist pricks my finger to check my blood glucose, and it’s good. Fine.
More scans. More pushing. This goes on and on and I lose track. Maybe that’s the Fentonyl. At some point the contrast is piped in too, to give a clearer image. Eventually, Miltos announces that we are ‘ready to ablate the tumour’.
At this point I get another dose of Fentonyl, and I’m not quite clear how this works. I don’t think that you are technically knocked out, but you’re knocked out enough not to know what is happening, or at least not to remember it, which will do.
So, while I drift off, they finally actually cook my offal. Which I was wearing at the time. And I wake up on the ward.
(Part 2 of Ablation Day will follow. I’m a bit knackered.)
Day 32 (Monday 23 April 2018)
Up with a list of jobs to do today, before going into hospital tomorrow. But I had a frustrating morning and failed on most fronts. Mostly it doesn’t matter. Weirdly, I’ve been finding it difficult to remember what you’re supposed to take into hospital.
EasyJet, the saga continues
At about midday I had a call from an EasyJet chap. He started by hoping that my journey home was better…
So we talked about that a bit. (It wasn’t, in case you’re new to the blog.)
He genuinely seemed to want to understand what’s been happening, and to try and get to the bottom of it. He ‘got’ that an apology was hardly going to solve the issue, wanted to know about other experiences, and if any other airline had a better model.
We talked around a whole number of issues:
- dignity;
- the ‘one-size-fits-all’ approach;
- staff assuming that they know what you need more than you do;
- the pointlessness of booking and logging information if it doesn’t get passed to the people who need it;
- the ever-present delays in off-loading;
- the routine non-arrival of promised wheelchairs;
- the constant worry, or indeed experience, of chairs being damaged and the awful consequences of that.
He seemed determined to try and instigate some changes. He seemed open to the idea of involving users properly in the design and planning of services. He wrote down ‘Plan with us not for us.’
Dunno. We’ll see.
Distractions
Friends came to see us in the afternoon, and we had a lovely couple of hours with them, sitting round the table eating cheese and grapes. I love tables.
I’ve been worrying, of course, about the procedure tomorrow. I have huge confidence in the Radiologist who’s doing it, and am trying not to think about the possible complications. But the risks are real, and potentially very serious. A significant bleed in the kidney, or other substantial damage, would likely lead to the loss of the kidney. And that would mean dialysis and a very serious curtailment of activities, spontaneity and so on.
I used to think that complications only happened to people who were old and sick going into procedures, and I’d ‘Yeah, yeah’ them away, like the people who can’t bear to watch safety procedures on aircraft. (More fool them.) But I learnt the hard way after the Whipple’s in 2011 that this isn’t necessarily the case, and I’m much warier now about the risks involved.
And on a pettier level I’m worrying in particular about how uncomfortable I know it will be, to have to lie on my face with my arms outstretched for, probably, about three hours without moving. My shoulders are stiff and sore already from lots of pushing lately. And an hour or so in, I know that they will be really very painful, with nerves feeling trapped, and I won’t have the option of moving anything to relieve that. So it’s going to be horrid, and I just have to grit my teeth and get through it. Like root canal.
A massage seemed like a really good idea. And tonight our friend and neighbour, Barb, slotted me in for quite the most marvellous massage I can remember. Right now my shoulders feel bendy and loose. Like new, or as though I’ve had a full service.
Nil by mouth after 2am, so I’m going for some porridge now.
Wish me luck. Back soon.
Day 31 (Sunday 22 April 2018)
Sunday at home. A glorious day, starting with French toast. You can’t go far wrong with that.
Then four of us gardening pretty much all day. After all that rain and a week of heat, the garden is… erm, lush. Weeds everywhere and everything going bonkers. Knee pads and sun hats. Steps to clear, gravel to de-weed, paving to scrape, roses to prune. Desultory conversation and refining plans for the wedding. Happy and companionable.
Lunch in the garden with long drinks. And more gardening. At the end of the day we don’t seem to have made very much impression though…
Then over to Wolverton for a most splendid dinner with good friends.
Gosh, but we were tired. I was driving, and had to stop in a lay-by for forty winks on the way home. Another late night!
A good day, with the young people and good friends. What more could you want?
Day 30 (Saturday 21st April)
Night mozzie log: one more bite.
Today is our last day in Nice. We’re leaving on a late flight at about 10pm, and decided that we’d go to Antibes for the day, by train.
After breakfast I packed. I always pack, partly because I’m a bit of a fascist about how it’s done. And partly because there is always the tricky gear conundrum. Today’s was about packing, then leaving the bags at the hotel, complete with separated liquids, separated meds, the pumps where they can bypass the x-ray machine, etc.

But I also needed to have some of this with me during the day, but organised so that it could rejoin the other gear and be processed by security at the airport. The back-up gear that’s usually stashed under my chair can’t go through security like that, and once I’ve got the Kevlar ‘trousers’ on my wheelchair tubing, to protect it from the baggage handling, I can’t get at anything underneath. So, just logistics, but it’s a bit of a faff.
Once packed, we hoofed up to the train station, and within half an hour, we were in Antibes, which is much flatter than Nice, and smaller. There was an art market, and squillions of yatchs, a busy and colourful old town, and a rather good lunch. Again. I got in the Med. Just up to my ankles, but it was nice to do that.
The train back was packed with sunburnt people.
We picked up our luggage from the hotel, and eventually found the airport bus, much further from the hotel than we’d been led to believe
The EasyJet Saga …
Went to check in, as requested, in spite of having checked in, in spite of having no hold bags, and in spite of having apparently established several times by now that we wouldnt’ need any help until we got to the gate. You have to go and let them pat your head.
I checked with the woman that I could keep my chair to the plane door/steps; that I wouldn’t need the ambu-lift, and could she double-check that I could get my chair back on landing. ‘Oh, of course’, she said, ‘there’ll be no problem with that’. They always do.
A little later a guy came to us in the departures lounge, and said he’d come to take us to the gate. When we got there, the woman on the desk looked at my boarding pass. I was within sight of the airplane door, now, with a man who’d already promised to take me right there and then put the chair in the hold. Fingers crossed.
So I thought I’d best check about arrival in Luton.
‘Can you double-check, please, that when we arrive in Luton, they will be able to deliver my chair back to me at the aircraft?’
‘Oh no, that won’t be possible. They can’t do that at Luton.’
‘Hmm. They can, and they have, many times,’ I suggested, politely.
‘You’ll be fine, they’ll get you an Ambu-lift.’
’No, that wouldn’t be fine. I don’t need and Ambu-lift and don’t want one.’
I suggested that she look at my notes on the booking again. And I told her that I’d had five or six previous conversations with people who had assured me that it wouldn’t be a problem at all, including over the last couple of days with Johan the CEO (or ‘his people’, at least).
She looked carefully at the booking notes, then said. ‘Oh, I see. Hmm, yes, well I’ll get on to them and make sure that that is what happens. It shoudn’t be a problem.’
So, again, the question: If she has to ‘get on to someone’ to make this happen, what was the point of the previous phone calls, the online forms, the subsequent conversations and the passenger information?
The nice man took my chair to the hold. We got on. After a bit, I collared a member of Cabin Crew, and asked if she could double-check that my chair would be returned to me at…
She smiled beautifully, interrupted me and said not to worry, because she was sure that the Ambu-lift was booked.
I genuinely felt like a voiceless piece of luggage at this point. It does often seem as though the corporate world really, really does think that ‘people like me’ are all the same, that we can’t think for ourselves, and that they know what’s best for us. And if we’d just shut up and be happy to be shunted around like inanimate boxes, everything would be hunkydory.
So, anyway, I explained, again. She went off to speak to the Cabin Manager, and came back to say that yes, in fact, they were clear about all that, and my chair would be returned to the stairs or door. There’ll be no problem with that.
After a quick journey, involving a heavy tailwind, and amazing views of lightning round the edges of Paris and London, we landed.
After a short delay the ambulift pulled up, and I could see my chair inside it.

I had a discussion with the Cabin Manager, called Adam. He was appalled. He checked the info on his manifest. It said
- Passenger can ascend/descend steps.
- Passenger can’t ascend/descend steps.
Remember Rrrrroben? Remember how I phoned him back to correct that, and how he said he’d corrected it?
(It’s folded up in the photo to protect the privacy of other passengers.)
That struck him as pretty nonsensical, and he wondered how anyone could have entered this information into the system. He said that he knew the system was rubbish because he always had terrible trouble booking the right assistance for his grandmother. And he also said that the infrastructure at Luton was poor.
He went to the Ambu-lift and argued for bringing the chair round to the stairs, and the Special Assistance staff agreed to this (but were presumably disgruntled to be dragged out unnecessarily). However, at this stage he was also told that this particular gate didn’t have a lift (or a working lift?), so we’d have to carry the chair up two flights of steps. Hardly doable with two cases and a bag. I can manage steps, but not while carrying a chair. So Adam was right about the infrastructure.
In the end, then, there was no choice but to use the Ambu-lift, yet again.
And you could argue that this may have been the reason all along for the difficulties – that there wasn’t really a choice given the liftlessness. But this wasn’t the reason. (Apart from anything else, the arrival gate would only be decided at the last minute, and most of them certainly do have lifts. We’ve used them many times.)
So, I ask again: ‘What is the point of booking special assistance, weeks ahead, with numerous people, and checking at every point on the journey, repeating over and over again what it is that has been specified and agreed, if the information isn’t passed to the appropriate places and acted upon?
The reason that this farce occurred, yet again, is that neither EasyJet, nor the airport, nor the Special Assistance providers actually give a toss about the quality of the journey that its disabled passengers experience.
They will protest and say that they do give a toss, and that they do care, but they don’t.
They know that this is what happens, over and over again. They know that the experience is dreadful because ‘the wheelchairs’ complain, and make concrete suggestions, and offer to help them to plan and design a service that would work. They know that the experience Frank Gardner made a fuss about is common. That waiting for an hour to get off a plane is common.
And, still, they choose to do nothing.
Day 29 (Friday 20th April 2018)
Four weeks today since my most recent diagnosis.
It all seems very strange. Here I am with H on the French Riviera, eating well, drinking the marvellous rose, watching tennis and the world go by. And just four days away from a cancer treatment that I wouldn’t have known I needed but for CT scanning technology. I feel fine and have no symptoms. If it’s all straightforward on Tuesday, by this time next week I’ll be right as rain and at the Eastern Blue Stars annual fundraising tournament.
We’re due a lovely day again.
I’m a bit cross, though, about being bitten twice by a fecking mosquito during the night. Once near my collarbone, and another on my forehead right between my eyes. That’ll grow during the day… That’ll look nice.
We get the No. 15 bus from just outside the hotel, up to the suburb of Cimiez, where the Musee Matisse sits in a lovely park. The museum is being refurbished, and quite a lot of it wasn’t wheelchair accessible, but we saw lots of Matisse’s work, especially his later stuff – the ‘Travail et Joie’ that I’ve always loved, and the very vibrant, colourful gouache paintings made from his paper cut-outs.
The colours make me happy. I’m basically twelve.
We had a simple lunch in the park, and sat under a tree for a while. A large and noisy group of Italian kids on a language-school holiday (who must have moved on from Cambridge, because you can’t move for young Italians there) provided two lasting images.
First, nine of them were sitting on a wall with their legs dangling down, and every single one of them was peering and keying into his or her phone. (These weren’t the noisy ones.)
Second, they were all having lunch provided by their tutor, via a huge bag of sliced spread, a blunt knife, and a colossal jar of Nutella. They seemed happy enough, but it’s hardly the Mediterranean diet you imagine Italian kids eating.
Afterwards, there was a bit of unproductive shopping on my part, during which I didn’t buy a dress in Desigual. That took some guts.
Later we met the guys again and, again, ate splendidly.
The EasyJet story continues
 Mostly because my good friend Steve provided the exact email address of Johan the CEO at EasyJet, and Ian (Director Customer) who, I’m sure, are both ‘working hard to make my journey comfortable’), have now been apprised of my miserable experience on Monday. I’d had an email insisting that they’d really like to know how my flight had gone, so I sent them a link to my blog and referred them specifically to Days 14, 18 and 25.
Mostly because my good friend Steve provided the exact email address of Johan the CEO at EasyJet, and Ian (Director Customer) who, I’m sure, are both ‘working hard to make my journey comfortable’), have now been apprised of my miserable experience on Monday. I’d had an email insisting that they’d really like to know how my flight had gone, so I sent them a link to my blog and referred them specifically to Days 14, 18 and 25.
An hour or so later I had an email from Johan’s Executive Assistant, asking if they could ring me to discuss this at some point. I said, yeah.
Then, while we were having a pre-dinner drink in Nice’s Place Massena, I got a call from ‘Tui’ ( a person not the holiday company) who works for Ian, who was calling to apologise for the awful experience. We couldn’t talk easily because we were in a noisy public place, but I said, more or less, that an apology was neither here nor there, and pointless, because I was likely to have the experience again and again. I suggested that the only good outcome would be if the experience were to change. And that this would almost certainly involve overhauling their systems and the contracts that they have with – or the influence they have over – the companies that provide the assistance.
Anyway, we’ll see where that goes. They’re going to ring on Monday when I’m at home. And in the meantime, she had phoned Nice airport to check the assistance that was booked there. We’ll see how that turns out.
I said ‘Design with us, not for us. Plan with us, not for us.’ That’ll ring a bell or two with some of you.
Day 28 (Thursday 19 April 2018)
A pretty relaxed day.
Breakfast was busy, with 40 hotel guests from an Arts Society in Surrey congregating for brekky before being hauled off to the Russian Cathedral in a bus. Earnest but lovely. Lovely but earnest.
We didn’t have much of a plan, except to stroll and wander. We spent a while people- and particularly children-watching at the lovely great avenue of fountains – the kind that stop and start and go small and tall. There must be a name for them. They’re a delight for adults, but it’s glorious to watch little children playing in them.
There were parents with kids who were obviously local, and who had been dying for the sun to come back after a long winter and the rubbish weather that they’ve had here. The kids peeled off clothes down to swimming togs, and shrieked in and out of the water. There was a boy of seven or so, obviously an old hand at this, who was showing his little brother how to have maximum fun. He jumped and danced and whooped for the best part of half an hour. I found myself really hoping that by next year he would still be this uninhibited about his delight.
Then there were the tots – either local or visitors – for whom this was new. They’d wander through the stopped phase, and then be startled, cautious, and highly amused, as the fountains came and went, and steadily grew into tall columns, or seemed to move about as some were still. They weren’t sure if it was okay to get wet, and were delighted when that turned out to be part of the game.
Through the Massena gardens and on down to the Promenade des Anglais, which we now, like old hands, call the PDA. And we had a drink on the beach.
After more of a stroll we decided to eat at one of the beach restaurants – all navy blue and white brollies, and blue sky and blue sea and white table cloths. Lordy, it was nice. So we had a pichet of rose wine (I can’t do accents on the Logitech keyboard), and ‘just a light lunch’ turned yet again into a monster meal with some of the best chips ever. During lunch we watched a pigeon called Gavin showing off with a twig to his Stacy.
‘Look, look! I can hold it at this angle!’
‘Yes, Gavin.’
‘Or this angle. Or this angle. And I can throw it up a bit and catch it. Look, like this! Look! Look at me!’
She wasn’t impressed.
This is the life. After this were so tired that we had to go back to the hotel.
I did a detour round a stationery shop and an art shop, and acquired some paper… God knows how I’m going to get it home.
And then back across town later to meet the folks for dinner, which we didn’t need. Peeling off my outer top in the restaurant, I realised that my Libre glucose sensor (see blogs passim) had come off my arm, and was loose in the top. So it was a good job I had the back-up pack under my seat, with the testing strips and the lancets and the lancing device, wasn’t it?
By the time we got back to the hotel I’d done 12,800 steps, according to my Fitbit, without even trying. Doing that many without having played basketball is a first. I should be fit going into this procedure on Tuesday!
Day 27 (Wednesday 18 April 2018)
Up in good time to go to Monte Carlo, to go to the Rolex Tennis Masters at the Monte Carlo Country Club.
There is a train service from Nice, but the French railworkers are on strike – good for them, we say – and there are no trains today. So we’ve booked a big taxi to take seven of us to Monte Carlo, and after breakfast I wait on the street for Jeremy, Hilary and Co. to arrive. (This is probably the only occasion in my life when I can do a ‘Monte Carlo or Bust’ joke.)
The other six folk were all installed in the back of the taxi, so I sat in the front with the very smartly dressed young driver, which was fine except that HE WAS TEXTING! As he got back in the taxi he sent a text, and I thought that was okay; probably letting the company know that he’d completed the pick-up. But he continued to text, in Nice itself – at lights, going through junctions, changing lanes – and then as we got onto the major, fast roads out of town. And he wasn’t just reading them, he was writing them too.
As we got onto the motorway I told him to stop. He seemed a bit surprised, and he looked a bit sheepish, as though he’d assumed I wouldn’t notice. Good grief. He did stop, but it made for a rather frosty atmosphere in the front.
Winding down from the motorway into the top of Monte Carlo is pretty stunning. You can smell the money.
We came here last year, to celebrate Jeremy’s ‘big’ birthday, and I’d contacted the ticketing office ahead of arriving, to ask how I could best sit with my friends, and have access to my wheelchair. Splendidly, they’d suggested that I could leave the chair ‘under the tribune’ (under the stand) while we were watching tennis. This worked wonderfully for most of the day. Then, during the afternoon, coming back from the loo or somewhere, a chap asked what I was doing, leaving my chair there, and said it wasn’t do-able, it was against the rules, that it (or was it me?) would represent a safety risk to other spectators, and…
You can probably write the rest yourself.
Fortunately I was armed with the email from the ticketing office, so after some further lively conversation with me and then with another member of staff, he grudgingly agreed to my leaving it where I’d just it it, safely tucked out of the way of anyone who needed the corridor or stairs.
So today I’m armed with a paper copy of this year’s email, agreeing to the same procedure, and wishing me a happy day. Ace.
Actually my ticket was for a single seat some distance from the other folk, because I’d bought it separately, so in fact, when the staff offered me a place in the court-side wheelchair area I decided to take it. Might as well be on my own there, than on my own in the gods. And then it turned out that a companion could come too.
The view was mostly great, although there was a period where we could only see half the court, because of a gaggle of press photographers. You’re really very near the players, and cheek-by-jowl with waiting teams of ballgirls and ballboys.
And there was a bit of shade, and we were very grateful for that. We could eventually make out the rest of our party in the huge stand, and found that they, like everyone around them, were gently wafting themselves with hats and programmes and fans. It was a slightly odd sight, like a wall of butterflies slowly twitching.
It was ‘only’ 23ºC, and it turned out that it was hotter in London, but the high surrounding stands, not to mention the high surrounding cliffs bounced the heat around like a small local sun, dedicated to the roasting of the Monte Carlo Country Club.

We saw Nisikori (No. 5 seed, I think?) play, then Djokovic. Next up was Nadal, whose knicker-fidging (is that just a family word?) provided splendid entertainment between the long ferocious rallies of baseline tennis. Then Cilic, too, although we had to leave partway through that to meet the taxi coming to take us back.
We were impressed that there were five women press photographers there. I’ve never seen this at other sporting events.
Nice dinner, weird service
We all ate together later on in a local restaurant who claimed to do the veggie/vega/gluten-free food that various people wanted or needed. And we had a rather strange experience. We were seven people, most of us rather ‘mature’ and wise in the ways of the world, which is to say fairly assertive. But, bizarrely, we were somehow collectively bullied by a strange waitress, who pretty much told us what to eat. She waved her hand at our vegan/veggie and told him: ‘I will bring you a plate of vegetables.’ Then she told Hilary, who really can’t eat gluten, that there was a particular thing she should have. And then when she brought the food out quite a lot of what arrived was very different from what was on the chalk-board menu she’d brought to the table. One chap ordered cod-steak risotto, and was a bit surprised to find no rice… He asked if this was the risotto, and she said ‘Yes, but we have no rice, so it’s leaks. But I haven’t changed the writing.’ And she pointed at the board again.
The food was perfectly all right. Just not what we’d ordered.
Then Howard and I walked back across town to our hotel, where I fell asleep fully dressed, apparently, and facedown on the bed. Howard woke me at 1am. I got up and folded all my clothes onto the shelves in the wardrobe, but have no recollection of this whatsoever.
Nice.
Day 26 (Tuesday 17 April 2016)
Nice
Woke up to sunshine in Nice, and spent the day tramping round the old town. Used the lift to get up to the old Castle Mount. The lift is built into an old well shaft. Stunning views and a beer at the top.
A late and long lunch in a square full of trompe l’oeil decorations. All those balustrades and pediments are drawn on. Like George Bush’s eyes – remember that?

The Fitbit saying 17000 steps at this point (pushes, not steps, natch). Back to the hotel and out again at 7pm to go and meet Hilary and Co. at an Italian restaurant.
A good evening. Good people. Then Jeremy turned up from the train.
Only twice, mid afternoon, and later after dinner, did it suddenly occur to me that in a week’s time I’ll be having a tricky day…
Oh, god, the glory of a little sunshine.
Nice. (I’m going to be doing that a lot this week.)
Day 25 (Monday 16 April 218)
A rubbish night after packing late, and not being quite sure that everything was in*. I woke up with a small dry cough about 3am, and wondered for a long time whether this meant that I needed to find antibiotics in the morning, before leaving at 9.15 for the train. Can’t turn up for an operation with a cough.
Nice but not Nice
Jim came to pick us up and took us to Bedford, to get the Gatwick train. What a star.
There was a right palaver getting on the train, with 6 elderly passengers who were going on some sort of church outing to Hassocks. They had about 53 enormous pieces of luggage, and two or three of them were very frail. It took four lift cycles to get them all on the platform. They were armed with those round tins of travel sweets, bless’em. But they were already fractious with each other. Gawd knows what they’ll be like after five days of praying…
Anyway, this was the easy part.
Look away now if you’d developed a soft spot for Rrrrroben.
I’d like Rrrrroben to be able to compare the journey through the airport that he imagined for us, with the one that actually happened today. It was beyond farce, beyond funny.
Special Assistance
On top of the emails spelling out what had been booked, I’d had a couple of messages on my phone, saying ‘Go to the special assistance area at the easyJet Plus bagdrop.’ And that we should make ourselves known to a member of easyJet staff.
(By the way, these camelCapitals are really getting on my wick now, so I’m going to call easyJet ‘EJ’ from now on.)
So, in spite not having a bag to drop, we went to the bagdrop area, and next to the bagdrop desks were two more desks with huge ‘Special Assistance’ signs on them. I ‘made myself known’ to a member of EJ staff, and she said that we should queue at the bagdrop to speak to the EJ guy working there, so that he could print me a luggage tag for my wheelchair, and that then we should go to Special Assistance on the floor above.
Not the Special Assistance just over there, next to the bagdrop, where I’d been told to go?
No, to the one upstairs.
In spite of two or three specific messages that said to report to this desk, next to …. ?
No. Go to the one upstairs.
Ok.
So we queued at the bagdrop for a bit to get the chair tag, but the queue, short though it was, wasn’t moving. Two women in Gatwick Handling uniforms were queuing too, and eventually they said that if I were only queuing for a chair tag, there was no need, and I should just ask the staff at the gate for one, later on.
So off we went upstairs. You’ll have noticed by now that our traipsing around in the big easyJet hall downstairs hadn’t achieved anything at all, and had wasted about half an hour.
Uptairs it took us ages to find the hardly-signposted Special Assistance area. God knows how visually impaired people track it down. To boot, it was at the very opposite end of the terminal to the bagdrop area downstairs. So the Fitbit, at least, is happy.
A guy there ‘logged me in’ and then told us that we would have ‘assistance through the airport’. I referred him to the extensive notes that Rrrrroben had made, and explained (again) that we didn’t need assistance through the airport, and (again) that the only assistance we would need at all was:
- getting downstairs from the gate to the apron (if, as is usual with cheap flights, there was no jetty),
- for someone to take my wheelchair from me at the bottom of the aircraft steps, and to stash it in the hold, and
- for someone to return said wheelchair to the bottom of the stairs on arrival in Nice.
Pretty much like a buggy.
Startlingly, his eyes glazed over and he lost interest about a third of the way through that, because ‘we only look after getting people through the airport here’.
He said we should:
- go through security,
- go to the gate an hour before the flight was due to leave, and
- tell the gate crew what we need.
Isn’t it a bit late, to explain to crew at the gate about the kind of assistance that you need??
What is the point of booking and specifying assistance online at the point where yo buy the flight, and then having phone conversations with SA staff ahead of the flight (‘We need at least 48 hours notice’, they say), if it’s down to a conversation that you have at the gate?
Security
Ye gods. As a diabetic, you need to be on the ball in airports, and especially in security.
Insulin cannot, not, NOT, NOT, EVER go in the hold, where it will freeze, and be rendered useless. And the pumps really MUSN’T through x-ray technology, because then they will be useless too.
The routine in security, therefore means that you have necessarily have extra liquids (insulin in vials and in cartridges, and also barrier sprays to reduce skin inflammation under adhesives), and you need to declare these meds, in addition to the bags of liquid that you’re already taking through (shampoo, cleansers, etc etc).
You also have to open and show staff the various bits of paraphernalia that accompany you everywhere (see Day 20 for more on this); point out the sharps (needles and finger-pricking lancets, including old ones that you might be bringing home); show them the hospital letter explaining that they really mustn’t put the pumps through the x-ray machine, and then watch like a hawk to make sure that they don’t.
Once, at Rome airport, the guy insisted that the pumps ‘would be fine’ in the X-ray machine. I said that they wouldn’t, and showed him the letter from the hospital (which you have to keep handy in case you run into tossers like this), and the manufacturer’s guidance that says that in no circumstances should this equipment be exposed to x-ray. Mr Tosser insisted that it would be okay. I insisted that it wouldn’t, and asked to speak to someone else, who obviously thought I was making a fuss, but who eventually promised not to put them through the machine.
While I was being frisked (I always am, because I can’t go through the x-ray doorway because I’m wearing a pump…), I looked round and saw that they had indeed put the gear through the machine. I howled at them and played bloody hell and created quite a scene. I was practically incandescent. If this had happened on the way out to Rome, we would have to have abandoned the trip and gone home. If you need insulin, you need insulin. There are no options. In Syria 10% of the population has diabetes, and they aren’t getting insulin, and they are dying.
Then as they are loading the plane, you have to make sure that your cabin luggage isn’t nominated for removal to the hold (where the insulin would freeze) as overflow luggage when the crew calculate that the overhead lockers will be too full. This is quite likely to happen, because you’re often the last person on the plane.
Anyway, in Security today I had quite the heaviest going over I’ve ever had. Every single items in my meds bag, in my under-the-seat pack and in my tool bag was individually unpacked and hand-scanned. The staff were lovely, in fact, and the guy doing most of it turned out to be a pump-wearing T1. They were just being careful, and that’s okay. But it’s slow and stressful.
Post security
We’d been told to go to the gate an hour ahead, but an hour ahead the gate hadn’t been called and we were hungry, so I went upstairs to Pret for a couple of sandwiches (other sarnie providers are available.), and while I was there I was summoned twice on the Tannoy (apparently, although I didn’t hear it), asking me to report to the Special Assistance area.
Wasn’t this way back past Security? How were we gonna get there? We were wondering about this when we realised there was an air-side Special Assistance area nearby, so we went and reported in, and were received politely, but as though we were naughty school children. No one had previously asked us to present ourselves at this place.
A woman called Sue told us that we would need to go with her, and another guy, to get on a bus to get the Ambu-lift.
Oh dear.
Why?
A long conversation ensued, about what had previously been agreed and written down, but none of it counted for Jack Shit.
It turned out that, because there was ‘another wheelchair’ who did need the Ambulift , and who would need escorting via a special, mystery gate (Gate 45L, who knew?), there wouldn’t be a member of staff available to escort me in the lift to the apron at the actual gate that our flight was leaving from. So, because we are all basically seen as pieces of luggage, we’d have to go this way too.
I acquiesced, mostly because ‘the other wheelchair’ was a bit embarrassed. We went on a magical mystery tour through back corridors, and emerged at a Gate 45L, where a couple of under-occupied and bored staff grudgingly issued a tag for my wheelchair. I asked them to make sure that the tag would specify that my chair would be returned to me at the bottom of the steps…
Then Sue handed us over to the guy in the crip bus.
Willy driving
After a palaver loading us into the bus (I climbed in, then Mr Driver used the ramp to lift my empty in after us, in spite of it only weighing four kilos), Mr Driver took us to the usual front steps of the aeroplane, where a strange, long ramp went to and fro up to the door of the aircraft. I’d never seen one of these before. It also had a short staircase at the back, which ground staff were using to come and go from the plane.
Mr Driver told us that we had to wait here until the Ambulift was available, at which point he would drive us round to the other (righthand) front door for loading. He got in and out a couple of times and had animated conversations with colleagues. Then Mr Driver took us the long way round the plane and parked near the front righthand door for a bit, next to the Ambulift, which was clearly there, but not available, while he had an exchange with the growing crowd of ground staff, who were obviously dealing with a seemingly intractable problem.
There was a lot of faffing about, and it gradually emerged that there were two ‘incoming’ families still on the plane (quiet a long time after everyone else was long gone), and that for some reason they couldn’t be disembarked.
Then he got back in and drove us back to the lefthand front steps. For a bit. We had been chatting to the other couple by this time, and it turned out that he didn’t need the Ambulift either, and would have been much happier just clambering up the stairs, like me. We explained this to Mr Driver.
In the meantime, one of the families emerged, and came down the long ramp with a fairly distressed young boy.
More ground staff appeared and there was a lot of arm waving. The lift was still round the other side and now the remaining incoming family could be disembarked. Our driver took us round to the Ambulift again, so that he could do that waving ‘left hand down a bit, straight on, STOP’ thing that they do, to help the lift driver connect with the righthand plane door. (He couldn’t have walked round there??)
Staggeringly, the Ambulift driver, meanwhile, was having a row with his dispatcher and was shouting into the phone in his left hand, and simultaneously waving his right hand around wildly as the Ambulift crept forward towards several million pounds’ worth of Airbus. My god! What the fuck was he steering with? I swear on all that’s holy, that he could only have been steering the lift with his willy.
I think at this point it’s safe to say that we were still in farce mode.
Now that the second family were disembarking we had to go back to the left side, in case we outgoing passengers accidentally mixed ourselves up with the incoming families, and by this time our Mr Driver was won over to our arguments that we could go up the stairs ourselves, as had been clearly and repeatedly stated (and recorded) in numerous conversation with everyone we’d jointly and severally encountered.
I’ve lost track a bit, now, and I’m sure that you have. And you have done well to make it this far. But at this point we went round to the righthand side again.
For a bit. Again.
Then we returned to the usual entrance and made our way up the ramp (we weren’t allowed to use the much shorter route via the steps, which was what we both would have preferred – because this shorter and easier route was for staff only!!)
I have to say at this point that our driver was actually good. He eventually got more or less what we wanted, in the face of opposition from the now-large group of ground staff advising and departing on all issues. He carried our luggage on, and took my wheelchair and put it in the hold. And he didn’t turn it upside down.
In the end the departure was delayed by 15 minutes, mostly caused by the incoming folks. It’s worth noting here, that from arriving at the airport to leaving on that old jet plane was two and a quarter hours, during which we experienced a maximum of 10 minutes ‘at leisure’, which we spent buying a sandwich. ALL the rest was sorting assistance. Ironic.
During the flight, as usual, I asked the cabin crew to please ensure that my wheelchair was returned from the hold to the aircraft door on arrival.
Nice but not nice
At the other end, ground crew entered the aircraft. I asked if my chair was coming to the door.
What chair? They weren’t expecting a chair to be delivered to the door. There hadn’t been a request or any information abou it.
There was a bit of an argument.
The chap from the Nice ground crew tried to help, and as I looked out of the plane and saw the luggage handlers put my chair on the luggage trolley with all the cases, upside down, he rushed off to try and intercept it, but failed. I banged my head repeatedly on the window at this point.
So, in spite of:
- two long phone calls,
- several online forms, and
- at least five conversations at the airport and during the flight,
(all of which ended up with agreement that delivering my chair to the aircraft door wouldn’t be a problem) my chair didn’t arrive at the aircraft door, and I ended up being pushed though the airport in a sort of wheelbarrow.
This isn’t an unusual experience. This is absolutely typical of the experiences we have at airports, at both ends of flights.
So, the question of the day is: ‘What is the point of booking Special Assistance if the specified and agreed assistance doesn’t arrive, and what does arrive is generic and designed for ‘People like you’?
And…
… breathe.
Post Script
On the bus into Nice, at about 6pm, I remembered that I’d spent ages awake with a cough last night, and worrying about a chest infection. There has been no sign of that today.
*It turned out everything wasn’t in. I forgot the European adapter (‘cos I’ve hardly ever travelled in Europe before. Not.)
Day 24 (Sunday 15th April 2018)
(Written on time, but posted late due to lack of internet while travelling)
A sound night’s sleep in Nottingham for me, between the two final games of our Women’s League season. Can’t say the same for my poor room-mate Eve, who says I ‘snore quite loudly’. We weren’t due to play until after lunch, so I met my old colleague and good mate Clare for brunch, and had a glorious catch-up.
Wheelchair basketball
Then to the Wildcats Arena, where I played the whole of a match again, against the same team that beat us yesterday. Our main strategy was hoping that they would be over-confident and manifest themselves as slackers, but it didn’t pay off.
Nah, that’s not true about it being our only strategy. We’re all playing better than we were last year, and we’re playing together better than we ever have. Emily has slowly and gradually (not to say painstakingly) made us into basketball players, and into a team, and we went onto court with a plan and with clear objectives.
Numbers, size and points
But the team is struggling in the division, in part at least because there are only six of us. This means that we aren’t able to play the ‘rolling substitutions’ game that many of our competitors play, and most of us play either for the entire match, or for a huge chunk of it. (I love this, and can’t get enough, but fresh hands can be a godsend in a hard-fought match.)
Being only six also means we are collectively paying only a small amount of subs, so our resources for kit and hall-hire time are very restricted. And, given that we are spread over the whole of East Anglia, it’s hard to persuade companies to sponsor us as a local good cause, because we aren’t really local to anyone.
And then, as well as being a numerically small team, we are also physically small. If you know me in person, you’ll get the drift if I tell you that until a few months ago I was our ‘tallest’ player by quite a stretch. This was a pretty weird situation for someone like me who has, forever, been the butt of all the small jokes. (I don’t always ‘get’ them, of course; they tend to go over my head.) Now, though, we have Eve, who is perhaps a whole inch (maybe??) taller than me.
Eve and I have have the highest reach, but really, we’re small fry. Most teams have a couple of big, properly tall players, who, for the most part, tend to be the goal scorers. These guys can catch and shoot over our heads, while we absolutely can’t shoot over theirs.
But we face an additional challenge in that, on top of being numerically and physically small, we are mostly ‘low-point players’. This is about classification.
Classification
Like lots of disability sports, wheelchair basketball uses a system of classification. Every player is assessed (while they are playing, rather than on the basis of a medical examination), and allocated a classification according to their level of impairment, with the lowest being 1 and the highest (able-bodied players) being 5. There are half-points in between. I’m classified as a 3.5-point player.
During a match you always have five players on court, and you can sub players on and off the court on a rolling basis. However, you can’t put more than 14 points on the court at any one time, so one of the difficult things about coaching (on top of all the other difficult things about coaching) is that you need to know the points total of every possible combination of players you might want to put on court. There are penalties, obviously, if you put too many on.
And, as well as being, until recently, the tallest player on our team, I am also the highest-point player in the team, which effectively means the least impaired. We’re a team of low-pointers. In fact, no matter what combination of players we put on court, we can’t actually muster more than ten points. And even if we were to put our entire squad on court (which of course you’re not allowed to do), we still don’t hit 14. So, in points terms, we’re almost a whole able-bodied player down.
I’m not making excuses, honestly. But what I’m trying to say is that we are improving without a shadow of a doubt, and we are playing our hearts out, but it’s a bit of an uphill struggle.

Nevertheless, it was a fabulous weekend, with lots of laughs, and honestly, the whole set-up – our team, the men who come along and train with us, the people who come to games to support and carry water, the league itself, our wonderful friends and competitors – is just quite bloody marvellous. Thanks, too, to Chris and Sara who travelled to Nottingham just to cheer us on.
I ache all over this morning, but my smile muscles are the sorest.
Back home through sun, rainbows, and periodically torrential rain, to more shed improvements and what are now called cauliflower steaks and lentils. Can I just say we’ve been eating them quite a while and we don’t call them steaks? And I’d hate you to think that we eat them because they’re fashionable.
I should have started the clothes packing before 10.30pm, though.
Day 23 (Saturday 14 April 2018)
The less obvious impacts of cancer
Well, there are loads of them. Here’s one, for a start.
 This is me wearing a rat. It isn’t a real rat. It’s the trophy I was awarded tonight by my comrades in the Eastern Blue Stars Women’s Wheelchair Basketball team, for being ‘tit of the day’. Clearly, it isn’t a politically sound award, but it has the merit of being democratically awarded during dinner to the team member who does the most stupid thing on the first day of our weekend tournaments. I ran over the referee’s foot. You didn’t orta do that. So I had to wear the rat.
This is me wearing a rat. It isn’t a real rat. It’s the trophy I was awarded tonight by my comrades in the Eastern Blue Stars Women’s Wheelchair Basketball team, for being ‘tit of the day’. Clearly, it isn’t a politically sound award, but it has the merit of being democratically awarded during dinner to the team member who does the most stupid thing on the first day of our weekend tournaments. I ran over the referee’s foot. You didn’t orta do that. So I had to wear the rat.
When I was diagnosed with cancer in 2001, this wasn’t one of the consequences I envisaged. I worried about the usual things: the treatments, the pain, the loss, and a million other things. But it never occurred to me at that point that there might be silver linings, too – that I might end up wearing a rat and laughing uproariously with a group of people I have come to know and love through playing wheelchair basketball.
It isn’t all rats
When I was asked in 2012 if I would be prepared to talk to a group of Macmillan-sponsored GPs in London, about the less obvious impacts of having cancer, I said that I was sure that there were three or four things I could think of…
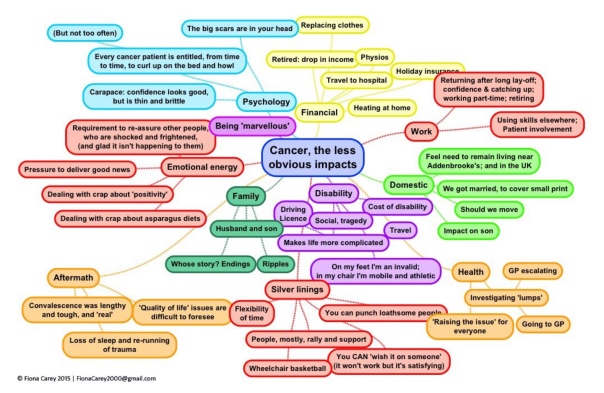
I sat down later that day and used a mind-mapping app that I used to use at work, to collect my thoughts. I was fairly astonished a few minutes later to have produced a mind map that completely filled an A4 page. The version below is a very slightly modified version of what I produced in those 15 minutes. I could add a bit more to it now, again, but I think that it’s pretty striking as it stands.
It’s been used in a fair number of places to trigger discussions, and if you want to use it, feel free to share it.
Day 22 (Friday 13 April 2018)
Developments on the orders front
Boots in Cambridge phoned last evening at about 6.30pm to say that my order of Freestyle Libres has finally arrived. They will be clearly labelled, and it won’t be a problem picking them up. Hmm.
This morning, Boots in Biggleswade phoned to say that the four I’d ordered there, would be delivered tomorrow morning (in much shorter order than had been the case in Cambridge).
Then the doorbell went, and a man in brown was holding the two I’d ordered direct from Abbott.
So, bloody hell, I’ve gone from a proper paucity of Freestyle Libres, to a serious plethora.
Next I picked up PDIL from Sandy, who was arriving to apply more paint to the shed. Then Ted came for a coffee with Ted, and was swiftly embroiled in the application of some guttering. And then I went off to Cambridge to pick up the order.
(And have a bitova look at some shoes to match El Frock.)
Later I picked up Eve, so that we can travel to Nottingham together tomorrow for National Womenn’s League Wheelchair Basketball. Really looking forward to that.
Then Frank arrived, and Howard cooked a sodding great oxtail, and we did what’s often best in the world, and sat round the table for hours, eating, drinking until late.
Day 21 (Thursday 12 April, 2018)
Tiny blog today. I get a day off, and so do you!
I wrote an email to the Monte Carlo Country Club (you don’t do that everyday) asking them if, while I’m watching the tennis next week, I can leave my wheelchair at the bottom of the steps under the stands, like I did last year.
This had been their suggestion, and it was a good job I’d got an email saying so, because – on the day – a jumped-up security bod insisted that it really wasn’t possible, and it represented a security hazard, and … Oh, you know, the whole usual story. Anyway, I had the email, and he had to back down.
I had a swift reply saying that this would be a perfectly good arrangement again, and wishing me a lovely experience. So that was nice.
Day 20 (Wednesday 11 April, 2018)
Long-blog warning.
The big job today – sorting diabetes gear for our Nice trip
We aren’t going until Monday, but I’m away all weekend playing women’s wheelchair basketball in Nottingham.
Managing my diabetes is the hardest thing I do. This post is about organising diabetes gear, rather than managing the diabetes itself. It isn’t as difficult, but it is time consuming and, like all aspects of diabetes, relentless and inescapable. The blog isn’t intended to be complainy, just an account of some of what’s involved. And remember, this is just the gear part!
I have diabetes directly as a result of my kidney cancer; I had Whipple’s surgery in 2011 to remove kidney cancer tumours from my pancreas. This involved extracting (technically amputating) most of my pancreas, part of my stomach, and quite a lot of other bits of offal (and also two lobes of liver, which turned out not to be cancerous), and it means that, amongst other effects, I have a lack of insulin.
The main gear
I use an Omnipod insulin pump system that’s fairly hi-tech. It comes in two parts. There’s the pump itself (on the left above – it’s about 6 centimetres long). It adheres to my abdomen or flank, has a canulla that inserts into skin, it is controlled by the ‘personal diabetes manager’ (PDM, on the right)) via Bluetooth. The PDM looks a bit like a clunky mobile phone, and it doubles as a Blood Glucose Monitor (BGM), so you can use it with blood testing strips and a drop of blood, to get an accurate reading of the glucose in your blood. Glucose monitoring, and its control, are at the heart of diabetes management.
It’s a great system and I’m lucky to have it. The pumps themselves are the ‘consumables’ in the system. When I need a new one (every three days), I peel the old one off, fill the new one with insulin, prime it using the PDM-BGM (which actually does a rather impressive 2,500 system checks during the minute or so this takes), then stick it on over some barrier spray.
 I also use a Libre ‘flash glucose monitor’, a lot of the time. A reader (on the right) scans a sensor that I wear on my arm, and reads a fairly constant flow of data about my glucose. (It measures interstitial glucose, rather than blood glucose, which is different, but I won’t explain that now except to say that it’s a close proxy, and good for most, if not all, purposes.
I also use a Libre ‘flash glucose monitor’, a lot of the time. A reader (on the right) scans a sensor that I wear on my arm, and reads a fairly constant flow of data about my glucose. (It measures interstitial glucose, rather than blood glucose, which is different, but I won’t explain that now except to say that it’s a close proxy, and good for most, if not all, purposes.
To keep this system going, you have to carry a lot of gear all the time. I once heard a bloke with Type 1 Diabetes (T1) say that he was enjoying a great day out, and having a fine time, when he realised that he must be dreaming, because he hadn’t got a rucksack with him. He was.
I should say, at this stage, and it’s important to remember, that we have it pretty easy these days compared with people diagnosed just a few decades a go. I met a man once, in his late sixties, who said that when he was diagnosed he was given some insulin, a syringe, a needle, and a metal file to sharpen it with! All this would need to be boiled repeatedly (several times a day, I assume) to make it sterile. And on top of that he was peeing into a test-tube and having to heat it over a flame to get an indication (not a very good indication, either) of the glucose in his blood. He had done well to stay healthy.
Day-to-day gear – what’s in the handbag?
On a day-to-day basis I carry much less than most people with T1 do, largely because I have always been hugely averse to carrying more than I have to. I’m still a relatively light traveller. But there is a minimum you need with you, and there’s no getting away from it.
This is the stuff in my handbag, and that I use all the time, day in, day out.
On the left, there is: the PDM, the flash glucose reader, insulin, , spare batteries, test strips, a lancing device, lancets. On the right, a box for sharps, sweets for hypos and snacks such as breakfast cereal bars to follow on with, to stabilise the glucose levels. The tablets are Creon, which is porcine digestive juices, and necessary whenever I eat because without a pancreas you’re also without digestive juices.
Also, you should always have a ketone monitor, which you need to use if your blood glucose is running very high. Ketones in the blood are very dangerous, and Diabetic Ketone Acidosis can kill you fairly quickly. If the ketones are running high you have to report to hospital, pronto.
Fortunately the Libre glucose reader doubles as a ketone monitor, as long as you’ve got the ketone-testing strips, so there are some of those in there, too
I check this stuff every day, and re-stock it where necessary. People who are less obsessed with travelling light might carry around large pots or packets of this gear, and won’t need to fill up so often. But not me.
Everyday back-up
But of course this isn’t enough, because if something goes missing or fails, or runs out, then you need back-up, and the amount you need is a combination of how far away from home you are, and how long you’re going to be away.
At a minimum, whenever I leave the house, I always have these spare things stashed in a pack underneath the seat of my wheelchair. If I didn’t keep it there, it’d have to be in a handbag or rucksack.
 Reading down the four columns: (i) barrier spray; a tube of glucose; (ii) spare pumps; more snacks; (iii) more sweets (Skittles or jelly beans!); insulin and alcohol wipes; buscopan in case of pain from adhesions; (iv) spare strips for my PDM, a lancing device, glucose strips and ketone strips that work in the flash reader when it’s doubling as a blood glucose monitor; and spare lancets.
Reading down the four columns: (i) barrier spray; a tube of glucose; (ii) spare pumps; more snacks; (iii) more sweets (Skittles or jelly beans!); insulin and alcohol wipes; buscopan in case of pain from adhesions; (iv) spare strips for my PDM, a lancing device, glucose strips and ketone strips that work in the flash reader when it’s doubling as a blood glucose monitor; and spare lancets.
The Libre reader provides another source of back-up, too, because as well as scanning for interstitial glucose it can also test for blood glucose, although it requires yet another kind of test strip to do so. So that’s three kinds of strips .
The eagle-eyed among you may be wondering ‘Shouldn’t I be carrying a back-up ketone metre, too?’ Probably, but I can’t be arsed, and you have to stop somewhere.
Packing for holidays
I think that packing for holidays is one of the single most stressful things I do. I’ve done it lots of times. (Lucky me! I have lots of holidays.) And I have checklists for different length of stay. But even so, I find it really difficult. There are lots of things to take and most of it has expiry dates, so you can’t just leave a pack ready to pick up and go. In addition, you need a lot of redundancy in the system, because if something breaks down you either need a spare, or something else to replace it.
The advice is that you should, for any trip, take at least twice as much diabetes gear as you expect to use, and that you keep it with you at all times while you’re actually travelling.
The big issue is providing redundancy in case something fails, or gets lost. You need back-up. And you kinda need back-up for the back-up. It can be hard to know when to stop with this. So you tend to take a lot of gear away with you, and bring quite a lot of it back, but you never know.
So what if stuff does fail?
If the pump itself fails, I always have spare pumps stashed in strategic places – in the car, in the pack under my chair. And I just change it for a new pump. (I’ll know about it because it gives off a loud beep, which gets louder and louder the longer it goes on.)
If the PDM were to fail it’s much more complicated, because it acts as a controller for the pump, and as a blood glucose meter. Unusually, I’ve got a spare PDM, and I keep its various programmes, targets and ratios synced with the ones on my main one, so that in an emergency I can simply swap to the substitute.
But if you haven’t got a spare PDM, and most people haven’t (and of course it might fail…), you need to have an alternative system for delivering insulin with you. So if you’re away from home you also need to have:
- syringes (two kinds for long-acting and fast-acting insulin);
- insulin cartridges (two kinds, as above) to fit the syringes;
- and a supply of needles (enough for 6-8 injections a day).
Oh, and a bigger sharps box for all the needles and lancets).
I generally reckon that if I’m no more than two hours from home, I’ll risk going without the needle system. But for trips of more than one night, this all comes too.
For five days in France, I’ll take this pack in addition to what’s in my handbag and what’s underneath my chair seat. Plus some paperwork.
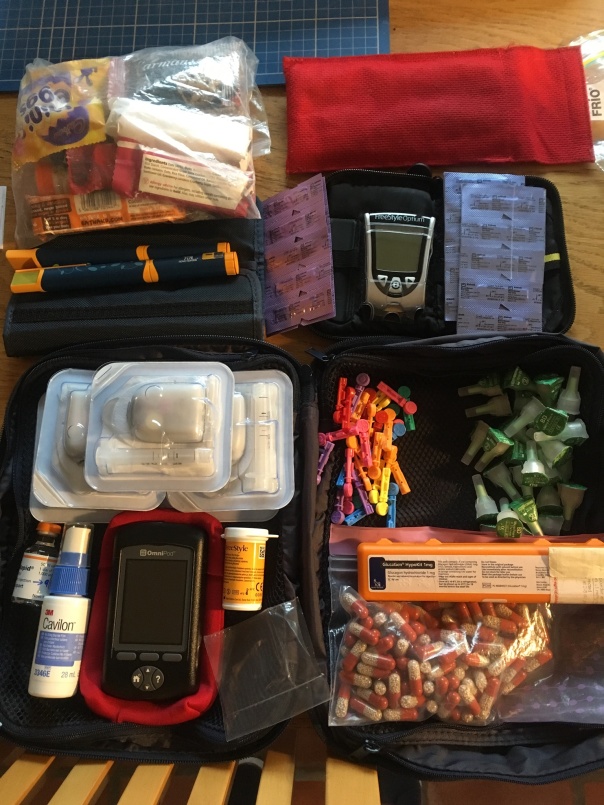
It’s mostly the same stuff in bigger quantities, plus the syringes, insulin cartridges and needles (the green vaguely conical things on the right), and a spare PDM. The orange box is a third syringe, this one pre-filled with emergency glucagen, in case of a serious hypo, so that Howard can administer if I’m unconscious. (Never had to use that, happily.)
The paperwork will include:
- a letter from Addenbrooke’s to show to security at the airport: to explain the sharps and allow them through the system; to show that the pumps musn’t be put through x-ray machines; and that insulin must not go in the hold (it freezes, and is rendered useless);
- a recent prescription;
- a copy of the fairly complex ‘Sick Day Rules’, which is a set of insulin protocols that you need to invoke if you end up with a high temperature or vomiting.
I’m also taking a copy of the letter from the hospital about the ablation on 24th, so that if I end up needing to come home early for any reason, I’ve got evidence of the need…
So, that should about do it. I’m wondering: Where do you stop? When is it irresponsible to skimp on gear, and just hope it’ll be okay?
In the end, I can’t cover every eventuality. If three bits of kit fail, I’m going to be buggered.
Should I be carrying a back-up ketone metre? Like I say, mostly I can’t be arsed, but when I go abroad? You bet. (Top right in the last photo.)
Gotta pack gear for Nottingham now.
Day 19 (Tuesday 10 April, 2018)
I did a long reading stint again between about half three and six this morning, but nevertheless feel a bit more like a human today,
The Grrrr factor continues
Can I say, first, that I genuinely feel for the poor sods who answer phones in customer service departments. But it is a strange and sometimes funny world of stock phrases and cliches.
I spoke again to Boots this morning, to a woman who spent quite a long time trying to identify the product I’d ordered. She kept asking ‘was it strips?’ and couldn’t quite believe that it wasn’t. When she finally went off to consult Sam, who had taken the order, she came back to say that he’d given up on Abbott delivering the order, and had put in a new order, which may take the now infamous ‘up-to-two’ working days. Not holding my breath.
Not going to Boots meant not going to John Lewis either, to pick up the stuff I’d ordered from them. So, worried that they might send this stuff back if it remained uncollected, I phoned them next. They, too, were experiencing high call volumes but I was deliriously reassured to learn that my call was important to them. ‘IF MY CALL IS SO IMPORTANT TO YOU WHY DON’T YOU EMPLOY ENOUGH STAFF TO ANSWER THE BLEEDING PHONES?’, I asked myself in a Zen-like state of calm (not).
Once through, they were nice enough, and having promised to hold on to the garment until at least Saturday, the woman sang the now-inevitable: ‘Is there anything else I can do for you today?’ I know they have to ask, but why would I be saying thanks and goodbye, if I still had an as-yet-unaddressed issue? (Yeah, yeah. I know it’s supposed to make me finish the call on a high and positive note, but it just makes me think the scriptwriter was stupid to assume that their callers are all that shallow.) Anyway, I made my now-inevitable riposte: ‘Oh yes, please. Can you do my ironing?’ There was a short pause, and she said she’d never been asked that before. Then she laughed like a drain.
So, next,with a heavy heart, I phoned Special Assistance at EasyJet. Unbelievably, my friend Robin (he is South African, so it sounds like Rrrrroben) answered the phone. Unfortunately, although I thought he was practically my best friend, he didn’t remember our call very clearly. Anyway, he acknowledged that the four bullet points didn’t appear to make much sense, but explained that each of them related to a different code, which summarised a set of assistance protocols, and would produce the right sort of help at the right point of my journey through the airport.
Sigh.
‘But,’ I pointed out, ‘the first says that I’m not bringing my own wheelchair, when I actually, really definitely am, and I don’t really get how even the most surreal protocol can interpret that as me “not bringing my own chair”’. Robin conceded that I might have a point, and now the first bullet point says ‘bringing own chair’.
‘And,’ I ventured, ‘I’m still troubled by the next two assistance protocols being mutually contradictory, given that one says that I can walk up and down stairs unaided, while the next is identical save for the word “can’t”’.
‘Ahh,’ he says, ‘the one that says “can’t” is there so that you’ve got the option of using the Ambu-Lift, in case – on the day – you can’t manage the steps. People do find that some days they can’t.’
Alarm bells. ‘People?’ (What people? Oh! People like like me? People ‘in chairs’. I’m so glad that Robin knows what we all find, and presumably how we all think and what we all might need. Oh dear… Someone else who knows about me and my disability better than I do.
‘But I will be able to manage the steps, Robin. I always can.’ See that? See what a nice bloke I am? I refrained from shouting ‘I KNOW WHAT I CAN DO BETTER THAN YOU DO!’
‘But this will give you the option, in case you can’t on that day.’
This went on for a bit, and I explained several times:
- That I definitely knew that I really, really wouldn’t need the Ambu-lift.
- That I also didn’t want to be kept waiting for the arrival of an Ambu-Lift that someone else had decided I might ‘need that day’. What? Are the cabin crew deciding that I look a bit peaky?
So… anyway, ’nuff said. Let’s just say that the bullet points no longer include the statement that I can’t do stairs. But Jeez. One size fits all, and we can either push you or lift you. It really is a like being a piece of baggage.
You know when people say ‘Life’s too short’? Well, sometimes it literally is, to be wasting time on crap like this.
Quote of the day
A friend who works in Oncology, and with whom I’ve done service improvement work, emailed to say that she had signed up to do Race for Life in Cambridge, so that we can do it together. She said, about the cancery news: ‘this just is not funny anymore is it?!’ I though that was spot on.
Day 18 (Monday 9 April, 2018)
Well, a day of ups and downs.
The Libre glucose scanner still hasn’t turned up At Boots, so my trip to Cambridge is off. Spoke to a different person today, and they didn’t seem surprised that it hadn’t come. Grr.
I also spoke to the Radiology Day Unit about the fact that I’ll be turning up later than their letter asked me to. The ward administrator was cool about it, and thought it was sensible. They won’t send out search parties if I’m not there at the crack of dawn. Or at least, they say they won’t.
On the EasyJet front, remember how optimistic I was after my conversation with Robin? Sure that he’d clocked all the right info…? I know I’m a fool, but I really thought this was sorted. But I opened up the information on our flight bookings today.
Under ‘Special Assistance and Nut Allergy Notification’ (which I’m assuming is a general heading, rather than an assumption about my diet), it says this:
- Not bringing own wheelchair (‘Oh yes I am!’)
- Can walk up and down stairs unaided (This is true, but the next one says…)
- Cannot walk up and down stairs unaided (‘Oh yes I can, and this is the exact opposite of the previous note.)
- Can walk around the cabin of an aircraft unaided (This is true.)
Good grief.
I know, I know. I shouldn’t have hoped. More calls tomorrow, then.
I’ve also applied to EasyJet for a refund on the flights we had to abandon, because of the operation. We’ll see how that goes.
I had another crap night, and have been awake since before 4am, but I’ve ‘done a bit of bookbinding’. I can handle it.
Day 17 (Sunday 8 April 2018)
Woke late and – apart from waking half a dozen times with hot flushes – felt as though I’d slept well. But I’ve been ridiculously tired all day. Couldn’t even address the book block I made yesterday. So, apart from doing a bit of cleaning and tidying, I’ve done bugger all.
H said, and I think he’s right, that this is basically how my cancerous state manifests. It’s a bit strange that, over its 17 or so years, the cancer has never actually made me feel ill. I did cough a lot before my first diagnosis (and I admit that I’d lost weight too), but it turned out that the coughing was due to the tumour pressing on my diaphragm, and that went away when the tumour was removed.
I coughed a bit again when I had a secondary in my lung, but really only a bit.
Apart from this, there has never been any of the usual signs of kidney cancer. No bloody urine, no difficulty peeing, no pain in the kidney.
And I’ve never had chemo, just surgery until recently, before adding ablation and radiotherapy into the mix in 2016/17, so I escaped the sickness and difficulties associated with chemo.
The only real symptom of the cancer is that I’ve been ridiculously knackered for years, and this seems to have got worse in the aftermath of the radiotherapy I had over that Christmas and New Year.
I know that people say it’s age, or that they’re tired too, but conversations with other cancer patients suggest that we do share a level of fatigue that is difficult to explain, and very difficult to cope with. I literally cannot remember last time I woke up feeling refreshed. I always wake up absolutely craving sleep.
I regularly do, and enjoy, high levels of activity. It’s important to keep fit, of course, and I like it too. And I can maintain a good thrash with the best of my basketball team. But the cost is high, and for a couple of days afterwards I’m so wiped out that I can’t really find words to describe it, as though someone has taken my batteries out, and I end up with days like today, when I just can’t rouse myself to do anything. I can’t concentrate, and I’m so tired I could cry.
Quite handy then, that my order of Libre glucose scanner, promised for delivery yesterday at Boots in Cambridge, still hasn’t arrived. Not sure yet if this is Boots being useless, or Abbott (the manufacturers) being useless.
Day 16 (Saturday 7 April 2018)
A rubbish night. (And here is a discussion-about-offal warning.)
Awake for a long time, wondering about the nature of this tumour ablation.
If the tumour is irregular, and you have to poke it in the middle, and radiate heat outwards, presumably that means that the process works best on a sphere. If it isn’t spherical – suppose its the shape of a kidney bean, or a raspberry, say – presumably you:
- either cook just the biggest sphere that you can, that is still contained within the tumour’s boundaries, necessarily leaving some edges with potential to re-grow;
- or you cook a sphere sized to encompass the whole tumour, with the inevitable effect of cooking some healthy kidney tissue around it. This is in rather short supply, of course, given that I’ve only got one, and that is already partly cooked.
Which means a choice between being cautious, going ‘small’, and you risk leaving mucky edges that can re-grow. Or you go for the whole thing and risk not only killing healthy surrounding tissues, but risking bleeding or damage to structures that you can’t actually do without, and which might easily lead to the need for dialysis. The tumour is just north of the central structure of the kidney, so this risk is reasonably high, and the reason that this procedure was preferred to open surgery.
So, assuming the conservative option, which is what’s been done before, it does look as thought this radiofrequency ablation might become a regular occurrence. It hadn’t occurred to me that the radiologist and I would become buddies.
I’ve felt properly knackered all day, from before I even got up. Frank and PDIL were still with us this morning – it’s wonderful having them around. They have breakfast with us, then depart early for Frank’s suit-fitting. This wedding is getting very real!
 H is still working away in the shed, and the stoopid cat got stuck on the new glass roof for ages. I’m feeling very unsociable and lethargic.
H is still working away in the shed, and the stoopid cat got stuck on the new glass roof for ages. I’m feeling very unsociable and lethargic.
Late in the afternoon, I sew a book block, ready for the next project. Then we eat and catch up with Scandy drama.

Day 15 (Friday 6 April 2018)
A solid sleep. Woke fogged and with swollen hand joints frI’m two days of training, then a day of cabinet building. On with the ibuprofen gel. Marvellous stuff.
Off to Cambridge in late morning with prospective daughter-in-law (PDIL), to try and buy a wedding frock via a John Lewis ‘personal shopping’ experience. I don’t like clothes shopping and hate all that dressing and undressing so the idea of someone who will find you clothes and keep fetching different sizes, while you only get undressed once seemed appealing. Even better with PDIL on board. And even better when they offered us a glass of Prosecco! Not me (I’mdriving), but PDIL’s eyes lit up. I’d warned them in the text box of the booking form that I usually dress like a twelve-year-old boy, while (unfortunately for them) having a pretty clear idea about the sort of frock I wanted. A bit underwhelmed at first by the PS woman and it felt like we were doing all the work. She also brought some jumpsuits, prompted by me (whey hey, nearly trousers), but the materials were pretty much crimplene, and terrible prints. One of them, navy blue with a little red and orange motif repeated at 4-inch intervals, looked like a sample pattern for a bus seat. Jaysus. But then PS woman came up with a Karen Millen frock that fits me like a glove, feels gorgeous, and makes me look pretty damned glamorous if you want to know. I love it.
Plus, there was a box of chocolates to take away. Next time you want pants, I recommend you book a personal shopper to help you choose them. Oh, and when she realised that I hadn’t had a Prosecco only because I was driving, PS woman gave me a bottle to take away!
What else? Phoned the Radiology Day Unit to tell them I would come in at 10 o’clock but the admin staff weren’t there, so could I phone back in ten minutes and in theory I could. But I forgot.
Day 14 (Thursday 5 April 2018)
Today, the sun shone. So that makes everybody feel better, innit?
I’ve spent this morning slowly sorting out alternative travel arrangements for our trip to France. A hotel booking I thought I’d made yesterday turned out not to have been book, so I had to start again. Anyway, the hotel is sorted now, and alternative flights booked for the Saturday before my ablation. That means we’re coming home a couple of days earlier than we had originally planned, and it’ll give us some breathing space. Happily the flight tickets for the Monday had been very cheap, and I’ve bought more cheap ones, so I thought it wouldn’t be a great loss just to ‘lose’ them.
I realise now that I’m relieved that we hadn’t booked to do this trip by train. Sorting out alternatives for that would have been a lot more complicated. I still need a conversation about special assistance at the airports, which I’ve been putting off since the original booking.
A letter from Addenbrooke’s confirms the arrangements for the ablation. As usual, it raises another question. The Radiologist has said (twice) not to arrive before 10 o’clock, because nothing will happen until then, but the letter repeats what’s in MyChart (the patient-accessible part of Addenbrooke’s Hospital’s records system), that I should arrive at 8.30am. I’m going to have to phone them and tell them I won’t be there until 10am, or else they’ll have me down as a no-show…
Then, a conversation with a splendid young South African man called Robin, at EasyJet’s special assistance line. Eureka! For the first-time ever, I felt I was talking to someone who could actually ensure that the assistance I need (minimal, much less than anything offered in their pre-defined combinations of assistance packages) might be available and actually be delivered. We’ll see.
He’s also added in a ‘medical bag’, so that all the extra gear I have to take for my diabetes won’t require us to book checked-in luggage. You always have to take (a) twice as much diabetes gear as you expect to use, (b) keep it with you, (c) make sure that no-one puts it through an x-ray machine (the pumps won’t work afterwards), (d) make sure that the bags don’t get ‘relegated’ to the hold, because insulin doesn’t work afterwards if it gets frozen… And stuff.
Airports are NOT RELAXED PLACES for me.
Anyway, he sorts all this without being phased, and then, on top of that, when I mention that we’d had to sort new fares and dates because of a hospital operation, he told me that they would almost certainly refund the cost of the unusable tickets. That seemed to me pretty much above and beyond…
In between times, three of us have been working in the shed, as part of the spruce-it-up project for the wedding. Less a spruce-up than a new-build, really, with H making new window frames, replacing glass, and making a new glass-covered ‘verandah’. So today we were painting, building cabinets, erecting wall panelling and running wiring. It’s going to be a mega-shed. We were inside the shed most of the time, but the prescience of glorious sunshine was bloody wonderful.
Then bookclub. Another group of brilliant women, and as usual we laughed and laughed. And we talked about the book, too.
Shame the fecking internet’s been down (here) all day since 3pm.
Mostly a good day.
Day 13 (Wednesday 4 April 2018)
We’ve got a date
I got a telephone message this morning from the Radiologist, confirming that he has made arrangements for the Radiofrequency Ablation (RFA) to be done on Tuesday 24 April. He has lined up the location, the people, the gear, the bed before on the radiology day unit, and an overnight bed in the urology ward. He’s done well.
Hooray!
I expected to feel relief, but I don’t think what I’m feeling is relief. I’m glad that he has managed to bring it all together, and undoubtedly relieved that the procedure hasn’t been pushed through to late May….
But, there are so many other issues.
First there’s the actual process, which will be unpleasant and painful. I’m already (still) having flashbacks to my earlier experience of it. The physical discomfort of lying stretched out on my front, arms above my head, and head turned hard to one side, for about three hours… Your shoulders really hurt after an hour or so, with nerves trapped and muscles screeching. Not to mention the additional discomfort of having a needle inserted and broddled about for a couple of hours. And the inevitable pain afterwards resulting from a sharp thing going through all sorts of tissue: it’s a kind of controlled stabbing. It’s not the sort of thing you’d pay for, unless you were a bit pervy.
Of course, then, I think that I should shut up and be grateful that these techniques are available. When my Auntie Winne died in 1968 (I think) of lung (or maybe oesophageal?) cancer , there weren’t many options. There was brutal surgery, then waiting until the mets caused enough havoc to produce symptoms again. There was primitive radiotherapy that burned you and scorched you and cooked delicate tissues. There were no scans, no subtle interpretation of digital imaging, none of the brilliant anaesthetics, no keyhole surgery. Auntie Winnie was a good human. (Also, she had amazing whiskers.)
Second, I’ve got to work out how I’m going to manage my insulin and my insulin pump during the three or four hours of the procedure which will, amongst other things, involve a dozen and a half CT scans. My insulin pump can’t cope with being scanned, so we have to sort out another way of controlling the whole set-up, and dealing with the high blood glucose that will, inevitably, be triggered by the psychological and physical stress involved. Bizarrely, I can’t remember what we did last time, so we’ll have to work it out again.
Third, should we cancel our trip to France? We’re due out on 16th and back very late on 23rd April, the night before the RFA. The flight is so late that if it is delayed there will be no way of getting back. Even the ‘Oooh could you get me on the next plane back because I’ve having a cancer operation in the morning’ argument won’t help if there aren’t any later flights. So I’ve spent several hours making arrangement to curtail the trip, and get us back on a flight on the Saturday.
I went to my women’s club training, where seven of us spent a couple of happy hours, tonking round the court, practising shooting, passing, curling, picking and generally taking the piss out of each other. We played a four-on-three game, the guys who come and train with us once again completely devoting the entire evening to the tactics we women need to practise in the run-up to next weekend’s competition. What peeps! What stars! I love these guys. I sometimes think that wheelchair basketball has saved my sanity. I certainly think it has preserved my health. It is bloody marvellous, and now my smile muscles ache.
Two other things.
- Looking back I realise that on five occasions today I told people that I was fine. I’m not really.
- Back home, we watched ‘Hospital’ on BBC. Look it up on BBC iPlayer, if you think you can bare it. This episode was all about managing cancer surgery lists in the absence of cancer surgeons, beds and, well, money.
I don’t really understand why we aren’t all out there ripping up the streets about the government’s systematic undermining of the NHS. How do we get people angry?
Day 12 ( Tuesday 3 April 2018)
It’s felt hard today.
I haven’t been able to concentrate on anything, and keep worrying about the timing of the ablation, and the follow-up, and its potential impact on our ‘summer activities’.
I wondered about calling the Marsden, to ask about the general possibility of having the ablation there, and what pathways and lead-times might look like. I got as far as looking up the department and the number but, for some strange reason I can’t put my finger on, I don’t have an appetite to do it.
But I’m fretting about when I’ll hear from Addenbooke’s about a date for the ablation. It’s a week now, since the Onc said that she thought the date was sorted subject to finalising some details, but I haven’t heard anything from anyone to confirm this (and she’s on a well-earned holiday, so I can’t ask her). I know it’s been Easter. But this is how time slips away. This is Day 12, and I’m basically no further on, I can’t answer any more questions, than I could on the day we got the news.
I assembled a cupboard for the shed project and made a couple of phone calls. But I’ve felt twitchy all day, and a bit teary to be honest. And I couldn’t decide whether, or when, or even where, to go shopping for some stuff I needed to put in the post. This isn’t like me.
Eventually I messaged the Radiologist who’s due to do the procedure, to ask whether there was any update about the arrangements, and he quickly replied that he’s ‘making arrangements for the 24th and will confirm shortly’.
This is actually a huge relief, to know that we are realistically looking at a date later this month rather than next month. But I also know that there are a lot of ducks to line up to make this a reality: places, people, gear, beds. And there’s also the possibility that this all gets lined up and booked, and that it still gets cancelled on the day. Who’d have thought, ten years ago, that we’d ever see a notice like this at a major hospital? ‘Hooray, we’re able to do cancer surgery today.’ It’s starting to feel a bit ‘third worldy’.

It’s made me think, though, that I probably won’t enquire at the Marsden. That’s kind of a relief. But this also means that I’ve got to steel myself for the RFA procedure to be done under sedation, which as I’ve said before, won’t be much fun. I shall just have to gird my loins.
Still, this way, if it happens, it’ll all be over by Walpurgis Night*.
Happily, my wheelchair basketball session tonight was really good fun. My Fitbit made fireworks because it was happy about the number of ‘steps’ I’d done today, and my colleagues there are such a good bunch of people.
* No, I didn’t know either but, as my husband often says, you learn something new every day. Walpurgis Night (Walpurgisnacht), is celebrated on April 30, the eve of the actual Christian feast day of Saint Walpurga , an 8th-century abbess in Francia.
* And you’re right; it won’t really be over by then, because there’ll be the four-week follow-up and anything else resulting from that. But the procedure, at least, will be done by the end of April. And I really wanted to tell you about Walpurgis Night.
Day 11 ( Monday 2 April 2018)
Time and luck
A slovenly start, after reading in bed, and dawdling over my private and shameful addiction, Killer Sudoko. Then lots of laundry after weekend visitors.
I’ve finally signed up for the Race for Life 5k, in Cambridge in July. Ironically I’d decided to do it a couple of days before I had the scan. I’d done it several times years ago, but had got out of the habit. I’m delighted that I’ll be doing it with friends, some old and some new. We aren’t going to be winning any medals I don’t think (although I did once ‘win’ the wheelchair race, on the grounds that I was the only one doing the event in a wheelchair.) It’ll be a hoot, and I’m already looking forward to it.
I’ve also been chasing people to play in my women’s wheelchair basketball fundraiser at the end of this month. Rellies, friends and colleagues coming to play basketball in our wheelchairs. It’s all a bit chaotic. A phantasmagoria of blisters and grinning.
And I’ve been finishing off the boxes I’ve been making on and off over the weekend, a spin-off from the bookbinding that I took up last year. Another addiction. ‘So I do a bit of bookbinding. But I can handle it.’ Remember that? Quite pleased with them.

I’ve also been wondering a bit about the business of time and luck.
It occurred to me that if I’d known in 2001, and certainly after my first diagnosis of metastatic cancer in 2003, that I was still going to be around in 2018, I’d have done a lot less worrying.
I wouldn’t have worried about surviving the lung secondary in 2003, for instance. When that was diagnosed I was really shocked because we’d persuaded ourselves – two years from the initial diagnosis – that the kidney cancer thing was all behind us. My friend Jane came up from Devon to see me, and helped me paint the living room (she’s quicker; I’m neater), and I cried for hours into the paint, terrified of the idea of wasting away in a hospital bed.
But I’ve had six diagnoses now. And I suppose that if someone told me tomorrow that I was going to have another six (and another 17 or 18 years??), that would seem like quite a good deal. I’d probably take that!
Or maybe I shouldn’t. May be I’d be short-changing myself? Perhaps I’m destined for a properly long life, and the cancer will be a continuing nuisance, that’ll just involve a lot of inconvenient episodes of oncological interventions, but leaving me plenty of time to have fun in between, playing wheelchair basketball; travelling with Howard; eating good food and drinking wine with friends; and eventually teaching the eventual grandchildren how to mix a proper White Lady.
Either way, I wish that in 2001 and again in 2003, and through the seventy-odd scans that I’ve had over the years, every one of which has driven me half crazy with fear, I’d known it would be a long job. The longer the better.
Everything is relative…
Day 10 ( Sunday 1 April 2018)
A fairly decent night’s sleep, after going to bed late.
I couldn’t sleep straight away. As soon as I lie down, stuff just goes through my head, over and over. So I read a while, and finally dropped off.
I had more hours of asleep than usual, but it’d be nice to wake up feeling refreshed. I never do.
My blood glucose has been good for a couple of days, mostly, and wasn’t bad overnight. In a previous bout of kidney cancer, in 20011, I had secondaries in my pancreas, and had most of that removed in a complicated surgery called a Whipple’s procedure. This, in turn, means I don’t have insulin, or very little (you can’t really measure or, more importantly predict – how much you continue to make).
So, without insulin, I have diabetes: not actually Type 1, because that’s an immunological condition, whereas mine is surgically induced, but my diabetes behaves exactly like Type 1, with the insulin, the carb-counting, the glucose measuring, the hypos and the worry about the long-term complications of having high blood glucose at least part of the time.
Blood glucose is really affected by (amongst other things) stress – physical or psychological. So, ho HO! Not much of that round here. Even just being in a meeting for half a day can make glucose run high, because of factors such as being more alert, keeping tabs, trying to ensure a good outcome. This is because the elevated cortisol impedes the effects of insulin, and so leads to higher glucose levels.
So, you can appreciate that with another diagnosis, comes another period of difficult glucose levels. It’s been tricky, but it seems to be settling a bit.
We have had a good day, with old friends over for lunch, great food, a little vino, lots of distraction and laughing, and some planning about the wedding in June.
But now, it’s starting to feel a bit like limbo again. I bloody well hope we get some news after the bank holiday.
Day 9 (Saturday 31 March 2018)
A bit of a rubbish night again. Thank heavens for the Kindle in the small hours.
I make a biggish breakfast, and the others come in from working in the shed to eat it.
I am really knackered today, and I think it’s just because my head is tired. I keep doing stupid things: I left the coffee machine running, until its tank emptied and the whole worktop was flooded. Can’t remember anything I’m told, or the answers to questions I asked a minute before.
Yesterday I cut board and did some prep for a box-making session (I have a bookbinding/box-making hobby-cum-habit) and today I started to put the trays together, which stopped me falling asleep. I hate sleeping during the day.
At some point we debate a bit about whether we can eat Easter eggs yet. We are all rabid atheists, and the debate doesn’t take long. We eat eggs.
I make some progress with the boxes.

What a bloody, wet day, though. Could do with a bit of sunshine. We’d all feel better for a bit of sunshine. Hard to believe it’ll be April tomorrow.
Day 8 (Friday 30 March 2018)
No news about scheduling, so I think that’s it on that front until Tuesday.
But a great day with Annie and Clare having arrived last night, and Frank and Bryony coming later. Frank and Bryony are helping with Howard’s shed project – part of the gearing up for their wedding.
A lovely, relaxed (Good) Friday afternoon. Nothing much, but chin-wag and laugh. And we didn’t crucify anyone, so that was good.
A little wine slipped down, and there was Cloud Atlas, and cocktails… then an amazing Chinese dinner by Howard.
Day 7 (Thursday 29 March 2018)
Even less to report. This is disappointing right now (although little to report CAN be a good thing).
Good things today
- Flowers!! I know I said not to, but two bunches of glorious flowers arrived today, and I have to say that they lift the spirits. And they smell nice.
- Late this morning my cousin phoned from Bath, and declared she was bored. I said ‘Come and see us’, so she (and her partner) got in the car, and did!
- They were at home when I arrived back after interviewing all afternoon for patient representatives to be part of the East of England Clinical Senate Council, of which I’m a member. The interviewing went pretty well, there were some useful candidates, and I was working with good people.
- H cooked a lovely meal (no change there, then) and we spent the evening chatting and laughing. We are supported by so many good people.
Less good things today
- I didn’t get round to contacting the Marsden, because this morning I was so tired and lazy after a bad night on Tuesday and a full day yesterday. And this afternoon I’ve been interviewing.
- I did spend the entire day, from waking until the evening, checking for more communications about a date for the RFA procedure. Can’t help it.
After thinking yesterday that something had been half-way organised I was hoping to hear a firmer date. - But no information has come through, so I have no idea whether the RFA might happen in late April, or late May… I completely get why it might not be possible to identify a date right now. I understand how hard it is to schedule locations, beds, people and gear. (There’s a lot of gear.) So I’m not blaming anyone. But now, with the bank holiday, it looks as though it’s going to be at least Tuesday before we know anything more. And that’s a good four more days of fending off the enquiries from well-meaning people.
- My blood glucose is creeping up. An undeniable sign of stress.
- I’m a bit weary.
Day 6 (Wednesday 28 March 2018)
Not much to report, today.
A very crap night in the hotel before co-delivering a workshop on co-production to the East of England Clinical Maternity Network. Still awake at 2am.
During the morning, the Onc emailed to say she was glad that April 26 was arranged. This was the first I’d heard, and this was the date the Radiologist thought wouldn’t be available. So that would be good, but unexpected.
I’m not sure whether she’s mis-read an email I sent late last night (easily done, I realise, on re-reading it), or whether she knows something I don’t. I haven’t heard from the Radiologist. Further email from the Onc suggests that the Radiologist may have nailed the all-important booking of the CT suite, and be trying to sort out availability in the radiological day unit beforehand, and the overnight bed on the urology ward afterwards. Lining up the ducks. Such a lot to schedule. And that’s without the staff!
I love these guys, and the bloody effort they make.
I spend the whole day trying to stay awake and keep an eye on the email and phone messages, while discussing ‘barriers to co-production’ … My colleagues are so good at this stuff.
Don’t hear anything further. So, at 10pm, I’m not sure where I am. There are two issues: the timing of the procedure and the availability of general anaesthetic. Since the referral to London is untested, I’m wondering about trying to contact The Marsden tomorrow, to find out whether we can get an idea of what that pathway would look like and, crucially, how long it would take.
- If it turns out that the option at Addenbrooke’s is a two-month wait (late May), then it may be worth at least exploring the London option.
- But if a late-April date is on the cards at Addenbrooke’s, that might be the more attractive option, even if it’s under sedation rather than under general anaesthetic.
So, I know very little.
Let’s see what tomorrow brings.
Day 5 (Tuesday 27 March 2018)
My beloved Logitech keyboard seems to have given up the ghost, and it’s late, in another bloody chain hotel, so I’m going to keep this short.
The Onc phoned (I love that she does this – what a sensible way to communicate!), to say that the Radiologist would contact me about dates for the radiofrequency ablation (RFA). A productive conversation, as always, and she warned me too that Addenbrooke’s is under enormous pressure, with A&E stuffed, and elective surgery being cancelled all over the place. The RFA is a Thursday procedure. April 12th is full; we’re away on 17th; 26th might be a possibility…
The Radiologist phoned me later from his car, and we also had a useful (if crackly) conversation, the gist of which is as follows:
- I learned that having the procedure done under a general anaesthetic is no longer an option at Addenbrooke’s because it is too difficult and expensive to schedule the requisite two anaesthetists, so I can either have it done under sedation, or they can refer me to another hospital (probably London, perhaps the Marsden?) for it to be done under general.
- I asked if that would involve more delay (another referral, more scans, more decision-making, then scheduling??). He didn’t know because they haven’t done that before.
- If I were to have it done under at Addenbrooke’s under sedation (which is uncomfortable, to say the least), that would probably involve coming in in the morning, having it done at 1.30-ish, staying overnight on the urology ward, and going home next day. Okay.
- He said he’d continue trying to assemble a team, and to schedule a time in the CT suite, and get back to me.
Like a hero, he phoned me again – still from the car – to let me know that 26th April was looking increasingly unlikely. It was excellent that he did this, so that I didn’t spend the next 24 hours making plans (and telling everyone that I’d got a date). He’s going to look at May 3rd. (He isn’t around on 10th and 17th May.) After that we’re looking at May 24th, a bare two weeks before Frank and Bryony get married. The Radiologist doesn’t know this; I didn’t tell him.
He is trying really hard, but the scheduling is difficult, and it’s looking as though there may be a very dispiriting two-month wait for treatment.
- Perheaps we cancel our trip in April?
- Perhaps we investigate the London option anyway? Might the Marsden be able to schedule it sooner, even with re-doing appointments and scans?
- What am I going to do with my head?
Dunno. This is where we are, and we might have more information to work with tomorrow.
As everybody seems to be saying these days: ‘It is what it is.’
Day 4 (Monday 26 March 2018)
Today I’m having a filling repaired, and hoping that the Radiologist will call to discuss dates for the ablation procedure.
In the meantime, here are some uncomfortable facts. They aren’t aimed at anyone personally, and I really hope no-one is offended.
- I’m a bit tired of people saying that they ‘know I’ll get through it’.
They don’t know. I don’t know. I am planning on getting through this episode, assuming that a tricky procedure goes straightforwardly. But when you have cancer, getting through it isn’t a given, or a factor of how hard you’re trying. It’s mostly luck. - I’m weary of people saying I’m amazing.
I was given this; I didn’t volunteer. I’d pass it on if I could. (Honestly, I’ve got an eighteen-year-old list of people I’d give it to!) Right now, I’m just putting one foot in front of the other. - Having another diagnosis hasn’t become any less frightening just because it’s my ‘normal’.
I live on eggshells. I wear a carapace of confidence, like the beautiful iridescent shell of a scarab beetle. But at the first finger-ache, the slightest sign of nausea or pain in my guts or pelvis, the carapace shatters and cracks, like Tom on the wrong end of Jerry’s frying pan. Having done this five times before doesn’t make the shock of it recurring any less. In fact, it’s kinda the opposite. How many goes have I got?? - Actually, it IS grinding me down.
- I know you don’t know what to say. And I sympathize.
I know you want good news. I know that that’s because you love me (or at least like me enough to care) and you want me to be okay. But I also know that if I tell you bad news, you’ll be horrified. You’ll panic, and look round, and search for the good news. But sometimes the news IS just bad; sometimes the options are horrendous.
If you really aren’t sure what to say, best try ‘Have another gin?’ - I know that you’re glad it’s not happening to you. That’s okay.
- It feels as though I’m in the woods with a wolf, and some of the time he’s forgotten I’m there. Then he sniffs and remembers, and comes back hunting.
- New research I’m going to send to the BMJ. The amount of flowers and cards you get is in direct inverse proportion to the number of times that you have been diagnosed with cancer. I’m not trying to cadge gifts. But you have to admit that that’s pretty funny.
The Radiologist hasn’t called.
Day 3 (Sun 25 March 2018)
Two things
I realised I was awake when it dawned on me that I was thinking through the process of the radiofrequency ablation. It involves sticking a big needle through your lower back, and wiggling it upwards into the exact middle of the kidney tumour, which is frankly quite a long way. And for success, this needs to be done without hitting the diaphragm or puncturing the lung, or the bowel or other bits of GI tract; or skewering a blood vessel, or a nerve; and without wrecking healthy kidney tissue. Then, once it’s in place, a probe goes through the needle, into the tumour, and the probe is heated up via the mysteries of radio waves, where it kills the tumour with the heat from the inside, but without damaging healthy kidney tissue, natch. [Apols to skilled medics, for simplifying your hard-won skills.]
It’s less risky than open surgery, but it’s still risky. It occurred to me that, like Buzz Lightyear’s flying, this is basically controlled stabbing, topped off a bit of focussed cooking.
The other thing is that one of the completely, utterly, exhausting things about being in this situation, is the time and energy you spend re-assuring other people that ‘Yes, it could be worse; and yes, it should be sortable.’ It’s partly my own fault; I suppose I don’t have to. But it’s difficult not to when people try not to reel at the news, and you can see them thinking ‘I’m glad this isn’t happening to me.’ And, really, who can blame them?
Years ago I freaked out a good friend by phoning up and excitedly telling him ‘the great news’ that ‘I only had secondaries in my lung’. The deathly silence at the other end made me realise that EVERYTHING IS RELATIVE…
Anyway. Let’s hope there’s a call from the Radiologist tomorrow. I expect he’ll ring while I’m at the dentist’s having a filling repaired.
Day 2 (Sat 24 March 2018)
After a surprisingly good night’s sleep, we laid some new flooring in the shed in the morning, then set off to visit friends in North Norfolk. I feel curiously flat and a bit numb about the new diagnosis. I’ve always been very open (talkative?) about my cancer, but I’m frankly tired of it, and bored with it. I’d told our son yesterday, and today told an old friend who asked about the scan result. I’ve spoken twice to my brother, too.
Our friend in Norfolk is an old hand at cancer and, like me has survived appalling surgery. We have an understanding, and of course we tell them about this. There is no horror; no drama; no throwing up of hands. Just quiet support, fairly outrageous black humour, and the amazing new garden to see. Oh, and coq au vin. And then some more vin. That’ll do.
Day 1 (Friday 23 Mar 2018)
An appointment with the Oncologist, nine days after my routine, 6-monthly scan.
The usual delays. I understand them – the need for staff to spend time with patients who are unwell, or are having difficult conversation, making difficult decisions. But wish that the rolling information about the delays were more realistic.
I’ve been on tenterhooks. Little pings of pain in my abdomen, an ache on waking. All feeding the paranoia familiar to cancer patients.
And all against a backdrop that involves a busy summer. Our son is getting married in June, and in July we are booked to go to our niece’s wedding in the Caribbean. We’ve had to book flights and accommodation for the latter, even though I can’t get insurance until late May…
The Onc comes in and apologises for the delay. Sits. There’s a bit of a problem.
This is the rollercoaster
This is how the ride goes:
There’s a problem – bad.
Bit of a problem – good.
There is re-growth in the kidney tumour that was diagnosed in July 2016, and which was twice treated using radio frequency ablation (RFA) in September and November that year – bad.
It isn’t entirely unexpected, because we know that it’s difficult to ‘cook’ the whole tumour without damaging surrounding healthy kidney tissue (which in my case is in somewhat short supply), but a bit disappointing – err… dunno
We can re-ablate it – good.
The procedure is much less invasive than open surgery – good.
There are still risks, of course, and it isn’t mostly how you like to spend a morning – bad.
Recovery is faster, too. Much faster – good.
It isn’t a ‘new tumour site’, so there is no ‘new cancer’ – good.
It could have been worse, of course. There could have been multiple tumours, all over the place. We aren’t there (yet) – good.
The Onc thinks that we might be able to do the ablation quite quickly. This would be a massive relief. It’d be good to sort all this out in time for the summer celebrations!
The Radiologist will call early next week to set up dates.
I wish it had been a clean sheet, though.
Feeling very flat.
Gotta make calls now, mostly re-assuring people. It’s exhausting.






 More tales of patient-centred carelessness
More tales of patient-centred carelessness


